Value of fibrinogen-to-albumin ratio in predicting the formation and prognosis of collateral circulation in patients with chronic complete coronary artery occlusion
-
摘要:
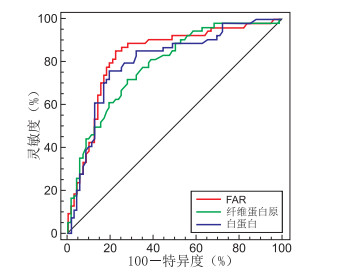
目的 探讨入院纤维蛋白原与白蛋白比值(fibrinogen to albumin ratio,FAR)预测冠状动脉慢性完全闭塞病变(chronic total occlusion,CTO)侧支循环形成及预后的价值。 方法 选取2017年10月—2019年4月在郑州大学第二附属医院择期行经皮冠状动脉介入治疗(percutaneous coronary intervention,PCI)术且至少1支主要冠状动脉CTO的冠心病患者126例。依据Cohen-Rentrop法将CTO患者分为侧支循环不良组(72例)和良好组(54例)。应用多因素logistic回归筛选评价CTO患者侧支循环形成的影响因素,采用受试者工作特征(receiver operating characteristic,ROC)曲线评价FAR预测CTO患者侧支循环形成的价值,以随访1年内主要不良心血管事件(major adverse cardiovascular events, MACE)发生率评价患者预后。 结果 侧支循环良好组患者FAR和高敏C反应蛋白水平均低于不良组(均P<0.001)。多因素logistic回归分析显示,FAR、高敏C反应蛋白与CTO患者侧支循环形成良好呈独立负相关。ROC曲线显示,入院FAR水平预测CTO患者侧支循环形成良好的曲线下面积为0.832(95% CI:0.755~0.893,P<0.001),诊断临界值为9.62,敏感度为85.19%, 特异度为77.78%。 结论 入院FAR水平对CTO患者侧支循环形成良好有一定的预测价值。较低FAR患者侧支循环形成更好,MACE事件发生率低,预后越好。 -
关键词:
- 冠状动脉慢性完全闭塞病变 /
- 侧支循环 /
- 纤维蛋白原与白蛋白比值 /
- 预后
Abstract:Objective To explore the value of fibrinogen-to-albumin ratio (FAR) in predicting the formation and prognosis of collateral circulation in patients with chronic total occlusion (CTO). Methods From October 2017 to April 2019, 126 coronary heart disease patients with CTO in an at least one major coronary artery were selected for percutaneous coronary intervention (PCI) in the Second Affiliated Hospital of Zhengzhou University. According to the Cohen-Rentrop method, patients with CTO were divided into two groups: poor collateral circulation group (n=72) and good collateral circulation group (n=54). Multivariate logistic regression screening was used to evaluate the influencing factors of collateral circulation formation in patients with CTO. The receiver operating characteristic (ROC) curve was used to evaluate the value of FAR in predicting collateral circulation formation in CTO patients. The incidence of major adverse cardiovascular events (MACEs) within one year of follow-up was used to evaluate the prognosis of patients. Results The levels of FAR and high-sensitivity C-reactive protein in patients with good collateral circulation were lower than those in patients with poor collateral circulation (P < 0.001). Multivariate logistic regression analysis showed an independent negative correlation between FAR, high-sensitivity C-reactive protein and good collateral circulation in patients with CTO. The ROC curve showed that the area under the curve of admission FAR level to predict the formation of collateral circulation in CTO patients was 0.832 (95% CI: 0.755-0.893, P < 0.001), the diagnostic threshold was 9.62, the sensitivity was 85.19%, and the specificity was 77.78%. Conclusion The level of FAR on admission has a certain predictive value for the formation of collateral circulation in patients with CTO. Patients with lower FAR have better collateral circulation formation, lower incidence of MACEs and better prognosis. -
表 1 侧支循环不良组与良好组冠心病患者临床基本资料比较
项目 不良组(n=72) 良好组(n=54) 统计量 P值 年龄(x ±s,岁) 67.3±11.8 62.4±12.6 2.221a 0.029 男性[例(%)] 42(58.3) 30(55.6) 0.097b 0.755 高血压[例(%)] 40(55.6) 29(53.7) 0.043b 0.836 糖尿病[例(%)] 26(36.1) 10(18.5) 4.680b 0.031 吸烟[例(%)] 38(52.8) 17(31.5) 5.690b 0.017 糖化血红蛋白[M(P25,P75),%] 5.6(4.9, 7.5) 5.0(4.8, 7.3) 1 409.500c 0.008 空腹血糖[M(P25,P75),mmol/L] 5.3(4.6, 5.8) 4.8(3.8, 6.3) 1 378.500c 0.005 甘油三酯(x ±s,mmol/L) 1.80±0.45 1.76±0.45 0.519a 0.605 总胆固醇(x ±s,mmol/L) 4.28±1.14 4.14±0.71 0.833a 0.407 LDL-C[M(P25,P75),mmol/L] 1.88(1.71, 2.11) 1.90(1.74, 2.39) 1 695.500c 0.220 HDL-C(x ±s,mmol/L) 1.45±0.38 1.37±0.26 1.306a 0.194 hs-CRP(x ±s,g/L) 4.89±2.17 2.75±1.82 5.869a <0.001 纤维蛋白原(x ±s,mg/L) 402.0±37.0 362.5±32.9 6.217a <0.001 白蛋白(x ±s,g/L) 37.0±5.2 43.2±5.3 -6.585a 0.001 FAR[M(P25,P75)] 11.28(9.96, 12.51) 8.31(7.28, 9.12) 653.500c <0.001 LVEF值(x ±s,%) 49.2±4.9 51.1±5.1 -2.097a 0.038 NT-proBNP[M(P25,P75),pg/mL] 238.5(88.3, 1 107.2) 100.3(43.1, 141.1) 1 264.000c 0.001 CTO病变部位[例(%)] 11.501b 0.074 左前降支 32(44.4) 24(44.4) 左回旋支 20(27.8) 18(33.3) 右冠状动脉 37(51.4) 15(27.8) 介入开通部位[例(%)] 4.788b 0.588 左前降支 30(41.7) 23(42.6) 左回旋支 18(25.0) 15(27.8) 右冠状动脉 35(48.6) 15(27.8) 1年内主要不良心血管事件[例(%)] 24(33.3) 9(16.7) 10.519b 0.044 急性心肌梗死 2(2.8) 0(0.0) 恶性心律失常 0(0.0) 1(1.9) 心力衰竭 8(11.1) 4(7.4) 复发心绞痛 11(15.3) 3(5.6) 心源性死亡 3(4.2) 1(1.9) 院前用药[例(%)] 阿司匹林+氯吡格雷/替格瑞洛 65(90.3) 49(90.7) 0.008b 0.930 β受体阻断剂 43(59.7) 41(75.9) 3.646b 0.056 ACEI/ARB 30(41.7) 23(42.6) 0.011b 0.917 钙离子通道阻滞剂 30(41.7) 15(27.8) 2.593b 0.107 他汀类药物 56(77.8) 42(77.8) 0.001b 1.000 注:a为t值,b为χ2值,c为U值。 表 2 CCC形成的影响因素多因素logistic回归分析变量赋值表
变量 赋值 CCC形成良好 是=0,否=1 糖尿病 是=0,否=1 吸烟 是=0,否=1 FAR 以实际值赋值 纤维蛋白原(mg/L) 以实际值赋值 白蛋白(g/L) 以实际值赋值 hs-CRP(g/L) 以实际值赋值 EVEF值(%) 以实际值赋值 NT-proBNP(pg/mL) 以实际值赋值 年龄(岁) 以实际值赋值 糖化血红蛋白(%) 以实际值赋值 空腹血糖(mmol/L) 以实际值赋值 表 3 CCC形成的影响因素多因素logistic回归分析
变量 β SE Wald χ2 P值 OR值(95% CI) FAR -0.676 0.171 15.691 <0.001 0.509(0.364~0.711) NT-proBNP <0.001 <0.001 3.561 0.059 1.000(1.000~1.001) hs-CRP -0.473 0.174 7.381 0.007 0.623(0.443~0.876) EVEF值 -0.110 0.069 2.530 0.112 0.895(0.782~1.026) 年龄 -0.027 0.020 1.698 0.193 0.974(0.936~1.014) 纤维蛋白原 -0.022 0.007 9.269 0.002 0.978(0.964~0.992) 白蛋白 0.141 0.043 10.773 0.001 1.151(1.058~1.252) 糖化血红蛋白 0.109 0.141 0.603 0.438 1.116(0.846~1.471) 空腹血糖 -0.518 0.244 4.499 0.034 0.595(0.369~0.961) 糖尿病 -0.751 0.440 2.917 0.088 0.472(0.199~1.117) 吸烟 -0.762 0.386 3.901 0.048 0.467(0.219~0.994) -
[1] SAXON J T, GRANTHAM J A, SALISBURY A C, et al. Appropriate use criteria and health status outcomes following chronic total occlusion percutaneous coronary intervention: Insights from the OPEN-CTO registry[J]. Circ Cardiovasc Interv, 2020, 13(2): e8448. http://www.researchgate.net/publication/339172014_Appropriate_Use_Criteria_and_Health_Status_Outcomes_Following_Chronic_Total_Occlusion_Percutaneous_Coronary_Intervention_Insights_From_the_OPEN-CTO_Registry [2] BHATNAGAR U B, NELSON G, STYS A. Collateral flow reversal: Exploring protective role of collateral circulation in acute coronary syndrome[J]. S D Med, 2019, 72(4): 174-177. http://www.researchgate.net/publication/334450857_Collateral_Flow_Reversal_Exploring_Protective_Role_of_Collateral_Circulation_in_Acute_Coronary_Syndrome [3] NIKOLAKOPOULOS I, VEMMOU E, KARACSONYI J, et al. Can history of myocardial infarction reliably indicate myocardial viability in patients with a corona ry chronic total occlusion and good collateral circulation?[J]. J Invasive Cardiol, 2021, 33(2): E135. doi: 10.1093/eurheartj/ehab724.1408/6393918 [4] CELEBI S, OZCAN CELEBI O, BERKALP B, et al. The association between the fibrinogen-to-albumin ratio and coronary artery disease severity in patients with stable coronary artery disease[J]. Coron Artery Dis, 2020, 31(6): 512-517. doi: 10.1097/MCA.0000000000000868 [5] XIA M, ZHANG C, GU J, et al. Impact of serum albumin levels on long-term all-cause, cardiovascular, and cardiac mortality in patients with first-onset acute myocardial infarction[J]. Clin Chim Acta, 2018, 477: 89-93. doi: 10.1016/j.cca.2017.12.014 [6] HWANG K T, CHUNG J K, ROH E Y, et al. Prognostic influence of preoperative fibrinogen to albumin ratio for breast cancer[J]. J Breast Cancer, 2017, 20(3): 254-263. doi: 10.4048/jbc.2017.20.3.254 [7] TAN Z, ZHANG M, HAN Q, et al. A novel blood tool of cancer prognosis in esophageal squamous cell carcinoma: The fibrinogen/albumin ratio[J]. J Cancer, 2017, 8(6): 1025-1029. doi: 10.7150/jca.16491 [8] 韩雅玲. 中国经皮冠状动脉介入治疗指南(2016)[J]. 中华心血管病杂志, 2016, 44(5): 382-400. doi: 10.3760/cma.j.issn.0253-3758.2016.05.006 [9] EMET S, ELITOK A, ONUR I, et al. Endocan: A novel biomarker associated with well-developed coronary collateral circulation in patients with stable angina and chronic total occlusion[J]. J Thromb Thrombolysis, 2017, 43(1): 60-67. doi: 10.1007/s11239-016-1424-6 [10] DAI Y, CHANG S, WANG S, et al. The preservation effect of coronary collateral circulation on left ventricular function in chronic total occlusion and its association with the expression of vascular endothelial growth factor A[J]. Adv Clin Exp Med, 2020, 29(4): 493-497. doi: 10.17219/acem/104535 [11] ZHANG D P, MAO X F, WU T T, et al. The fibrinogen-to-albumin ratio is associated with outcomes in patients with coronary artery disease who underwent percutaneous coronary intervention[J]. Clin Appl Thromb Hemost, 2020, 26: 1076029620933008. DOI: 10.1177/1076029620933008. [12] 赵一品, 季莹莹, 王丰云, 等. 纤维蛋白原与白蛋白比值预测急性ST段抬高型心肌梗死患者梗死相关动脉自发再通的价值[J]. 中华心血管病杂志, 2019, 47(2): 123-128. doi: 10.3760/cma.j.issn.0253-3758.2019.02.009 [13] 廖照亮, 董海燕, 卢振产. 单侧大动脉粥样硬化型大脑中动脉闭塞侧枝形成的临床因素分析[J]. 中华全科医学, 2021, 19(1): 59-61. https://www.cnki.com.cn/Article/CJFDTOTAL-SYQY202101018.htm [14] ZHAO Y, WANG S, YANG J, et al. Association of fibrinogen/albumin ratio and coronary collateral circulation in stable coronary artery disease patients[J]. Biomark Med, 2020, 14(16): 1513-1520. doi: 10.2217/bmm-2020-0333 [15] KAYAPINAR O, OZDE C, KAYA A. Relationship between the reciprocal change in inflammation-related biomarkers (fibrinogen-to-albumin and hsCRP-to-albumin ratios) and the presence and severity of coronary slow flow[J]. Clin Appl Thromb Hemost, 2019, 25: 1076029619835383. DOI: 10.1177/1076029619835383. [16] 赵一品, 汤建民, 季莹莹, 等. 急性ST段抬高型心肌梗死患者入院血清白蛋白水平与梗死相关动脉自发再通的关系[J]. 郑州大学学报(医学版), 2019, 54(1): 68-72. https://www.cnki.com.cn/Article/CJFDTOTAL-HNYK201901016.htm [17] ARQUES S. Serum albumin and cardiovascular diseases: A comprehensive review of the literature[J]. Ann Cardiol Angeiol (Paris), 2018, 67(2): 82-90. doi: 10.1016/j.ancard.2018.02.002 [18] G K M, KUNDI H, K Z LTUN E, et al. The relationship between ischaemia-modified albumin and good coronary collateral circulation[J]. Kardiol Pol, 2018, 76(2): 370-375. doi: 10.5603/KP.a2017.0213 [19] DEVECI B, GAZI E. Relation Between Globulin, Fibrinogen, and albumin with the presence and severity of coronary artery disease[J]. Angiology, 2021, 72(2): 174-180. doi: 10.1177/0003319720959985 [20] SHEN Y, DING F H, DAI Y, et al. Reduced coronary collateralization in type 2 diabetic patients with chronic total occlusion[J]. Cardiovasc Diabetol, 2018, 17(1): 26. doi: 10.1186/s12933-018-0671-6 [21] LI Y, CHEN X, LI S, et al. Non-high-density lipoprotein cholesterol/high-density lipoprotein cholesterol ratio serve as a predic tor for coronary collateral circulation in chronic total occlusive patients[J]. BMC Cardiovasc Disord, 2021, 21(1): 311. doi: 10.1186/s12872-021-02129-9 -





 下载:
下载: