Diagnostic value of bronchoalveolar lavage fluid mGNS technology combined with inflammatory factors for chronic obstructive pulmonary disease complicated with fungal infection
-
摘要:
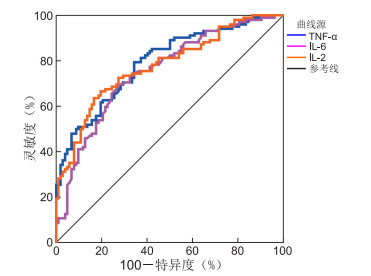
目的 为提高慢性阻塞性肺疾病(COPD)合并真菌感染诊断方法的准确性,针对当前传统诊断方法灵敏度和特异度均不理想的问题,本研究主要探究支气管肺泡灌洗液宏基因组二代测序(mGNS)技术联合炎症因子对该病的诊断价值,旨在为临床诊断提供可靠依据。 方法 选取2022年6月—2024年6月新疆维吾尔自治区人民医院收治的102例COPD合并真菌感染患者作为真菌组、102例COPD未合并感染患者作为无感染组。比较2组临床资料、炎症因子[肿瘤坏死因子-α(TNF-α)、白介素-6(IL-6)、白介素-2(IL-2)]水平,采用Pearson相关性分析研究炎症因子与肺功能[第1秒用力呼气量(FEV1)、用力肺活量(FVC)、FEV1/FVC]的相关性,采用ROC曲线分析mGNS、炎症因子对COPD合并真菌感染的诊断价值。 结果 真菌组糖尿病、低蛋白血症比例、血清TNF-α、IL-6、IL-2水平高于无感染组,FEV1、FVC、FEV1/FVC低于无感染组(P<0.05);血清TNF-α、IL-6、IL-2水平与肺功能均呈负相关关系(P<0.05);血清TNF-α、IL-6、IL-2诊断COPD合并真菌感染的AUC为0.793、0.754、0.778;mGNS诊断COPD合并真菌感染的灵敏度为91.18%,特异度为86.27%;mGNS联合血清TNF-α、IL-6、IL-2诊断COPD合并真菌感染的AUC为0.960,联合预测价值最大(P<0.05)。 结论 mGNS联合血清TNF-α、IL-6、IL-2在诊断COPD合并真菌感染中具有较高的临床价值。 -
关键词:
- 慢性阻塞性肺疾病 /
- 支气管肺泡灌洗液 /
- 宏基因组二代测序技术 /
- 炎症因子 /
- 真菌感染
Abstract:Objective To improve the accuracy of diagnostic methods for chronic obstructive pulmonary disease (COPD) complicated with fungal infections. In response to the unsatisfactory sensitivity and specificity of traditional diagnostic methods, the main focus of this study is to explore the diagnostic value of bronchoalveolar lavage fluid mGNS technology combined with inflammatory factors for this disease, aiming to provide a reliable basis for clinical diagnosis. Methods A total of 102 patients with COPD complicated with fungal infection admitted to the People ' s Hospital of Xinjiang Uygur Autonomous Region from June 2022 to June 2024 were selected as the fungal infection group, and 102 patients with COPD without infection were selected as the non-infection group. The clinical data and levels of inflammatory factors [tumor necrosis factor-α (TNF-α), interleukin-6 (IL-6), interleukin-2 (IL-2)] were compared between the two groups. Pearson analysis was used to investigate the correlation between inflammatory factors and lung function [forced expiratory volume in one second (FEV1), forced vital capacity (FVC), FEV1/FVC]. Receiver operating characteristic (ROC) curves were used to analyze the diagnostic value of mGNS and inflammatory factors for COPD complicated with fungal infections. Results The proportion of diabetes and hypoproteinemia, serum TNF-α, IL-6, and IL-2 levels in the fungal infection group were higher than those in the non-infection group, while FEV1, FVC, and FEV1/FVC were lower than those in the non-infection group (P < 0.05). The levels of serum TNF-α, IL-6, and IL-2 were negatively correlated with lung function (P < 0.05). The AUC of serum TNF-α, IL-6, and IL-2 for diagnosing COPD with fungal infection were 0.793, 0.754, and 0.778, respectively. The sensitivity and specificity of mGNS in diagnosing COPD complicated with fungal infection were 91.18% and 86.27%, respectively. The AUC of mGNS combined with serum TNF-α, IL-6, and IL-2 for the diagnosis of COPD with fungal infection was 0.960, and the combined predictive value was the highest (P < 0.05). Conclusion The combination of mGNS and serum TNF-α, IL-6, and IL-2 has high clinical value in the diagnosis of COPD complicated with fungal infection. -
表 1 COPD合并真菌感染与未合并真菌感染患者临床资料及炎症因子比较
Table 1. Comparison of clinical data and inflammatory factors between COPD patients with fungal infection and those without fungal infection
项目 真菌组(n=102) 无感染组(n=102) 统计量 P值 性别[例(%)] 0.188a 0.665 男性 62(60.78) 65(63.73) 女性 40(39.22) 37(36.27) 年龄(x±s,岁) 65.21±5.29 64.83±5.06 0.524b 0.601 BMI(x±s) 21.58±1.47 21.36±1.35 1.113b 0.267 COPD病程(x±s,年) 5.06±1.25 4.85±1.12 1.264b 0.208 基础疾病[例(%)] 糖尿病 38(37.25) 16(15.69) 12.190a <0.001 低蛋白血症 41(40.20) 17(16.67) 13.876a <0.001 高血压 33(32.35) 29(28.43) 0.371a 0.543 肺功能指标(x±s) FEV1(L) 1.04±0.21 1.36±0.30 8.825b <0.001 FVC(L) 2.03±0.24 2.32±0.33 7.178b <0.001 FEV1/FVC(%) 51.23±5.49 58.62±6.11 9.086b <0.001 炎症因子(x±s,pg/mL) TNF-α 44.96±9.38 35.20±7.42 8.242b <0.001 IL-6 9.58±1.41 8.32±1.18 6.921b <0.001 IL-2 252.77±32.15 225.06±24.63 6.910b <0.001 注:a为χ2值,b为t值。 表 2 TNF-α、IL-6、IL-2与FEV1、FVC、FEV1/FVC的相关性
Table 2. Correlation between TNF-α, IL-6, IL-2 and FEV1, FVC, FEV1/FVC
项目 FEV1 FVC FEV1/FVC r值 P值 r值 P值 r值 P值 TNF-α -0.682 <0.001 -0.703 <0.001 -0.714 <0.001 IL-6 -0.664 <0.001 -0.675 <0.001 -0.701 <0.001 IL-2 -0.637 <0.001 -0.652 <0.001 -0.685 <0.001 表 3 mGNS和传统病原菌培养的诊断结果
Table 3. Diagnostic results of mGNS and traditional pathogen culture
方法 类别 临床诊断(例) 灵敏度(%) 特异度(%) + - mGNS + 93 10 91.18 86.27 - 9 92 传统病原菌 + 77 20 75.49 80.39 - 25 82 -
[1] GBD 2021 Causes of Death Collaborators. Global burden of 288 causes of death and life expectancy decomposition in 204 countries and territories and 811 subnational locations, 1990-2021: a systematic analysis for the Global Burden of Disease Study 2021[J]. Lancet, 2024, 403(10440): 2100-2132. doi: 10.1016/S0140-6736(24)00367-2 [2] OTU A, KOSMIDIS C, MATHIOUDAKIS A G, et al. The clinical spectrum of aspergillosis in chronic obstructive pulmonary disease[J]. Infection, 2023, 51(4): 813-829. doi: 10.1007/s15010-022-01960-2 [3] KHANDELWAL A, CHAUDHARY S C, VERMA A K, et al. Nontubercular bacterial and fungal infections in patients of chronic obstructive pulmonary disease[J]. Ann Afr Med, 2023, 22(1): 77-81. doi: 10.4103/aam.aam_186_21 [4] COLOMBO S A P, HASHAD R, DENNING D W, et al. Defective interferon-gamma production is common in chronic pulmonary aspergillosis[J]. J Infect Dis, 2022, 225(10): 1822-1831. doi: 10.1093/infdis/jiab583 [5] TEKIN A, TRUONG H H, ROVATI L, et al. The diagnostic accuracy of metagenomic next-generation sequencing in diagnosing pneumocystis pneumonia: a systemic review and meta-analysis[J]. Open Forum Infect Dis, 2023, 10(9): ofad442. DOI: 10.1093/ofid/ofad442. [6] 中华医学会, 中华医学会杂志社, 中华医学会全科医学分会, 等. 慢性阻塞性肺疾病基层诊疗指南(2018年)[J]. 中华全科医师杂志, 2018, 17(11): 856-870.Chinese Medical Association, Chinese Medical Association Press, General Practice Branch of Chinese Medical Association, et al. Guideline for primary care of chronic obstructive pulmonary disease (2018)[J]. Chinese Journal of General Practitioners, 2018, 17(11): 856-870. [7] 中华内科杂志编辑委员会. 侵袭性肺部真菌感染的诊断标准与治疗原则(草案)[J]. 中华内科杂志, 2006, 45(8): 697-700.Editorial Committee of Chinese Journal of Internal Medicine. Diagnostic criteria and therapeutic principles for invasive pulmonary fungal infections (Draft)[J]. Chinese Journal of Internal Medicine, 2006, 45(8): 697-700. [8] 尚红, 王毓三, 申子瑜. 全国临床检验操作规程[M]. 4版. 北京: 人民卫生出版社, 2015: 69-71.HANG H, WANG Y S, SHEN Z Y. National clinical laboratory operating procedures[M]. 4th edtion. Beijing: People ' s Medical Publishing House, 2015: 69-71. [9] 李毅, 倪为波, 池毅, 等. 外周血NF-κB、IL-6、IL-10、IFN-α、T细胞亚群计数水平在预测AECOPD患者预后中的临床价值[J]. 中华全科医学, 2025, 23(4): 588-591, 690. doi: 10.16766/j.cnki.issn.1674-4152.003957LI Y, NI W B, CHI Y, et al. The clinical value of NF-κB, IL-6, IL-10, IFN-α and T cell subsets in peripheral blood in predicting the prognosis of AECOPD patients[J]. Chinese Journal of General Practice, 2025, 23(4): 588-591, 690. doi: 10.16766/j.cnki.issn.1674-4152.003957 [10] TOYCHIEV A, GAFNER N, BELOTSERKOVETS V, et al. Impact of Ascaris lumbricoides infection on the development of chronic pulmonary aspergillosis in patients with COPD[J]. Trop Doct, 2024, 54(2): 149-156. doi: 10.1177/00494755241226488 [11] LIU F, ZHANG X, DU W X, et al. Diagnosis values of IL-6 and IL-8 levels in serum and bronchoalveolar lavage fluid for invasive pulmonary aspergillosis in chronic obstructive pulmonary disease[J]. J Investig Med, 2021, 69(7): 1344-1349. doi: 10.1136/jim-2021-001857 [12] 王雅杰, 窦亚平, 高雪霞, 等. COPD合并肺部真菌感染患者血清学及肺功能参数分析[J]. 中华医院感染学杂志, 2020, 30(23): 3626-3630.WANG Y J, DOU Y P, GAO X X, et al. Analysis of serological and pulmonary function parameters in patients with COPD complicated with Pulmonary Fungal infection[J]. Chinese Journal of Nosocomiology, 2020, 30(23): 3626-3630. [13] WAS ' KIEL-BURNAT A, OSIN ' SKA M, SALIN ' SKA A, et al. The role of serum Th1, Th2, and Th17 cytokines in patients with alopecia areata: clinical implications[J]. Cells, 2021, 10(12): 3397. DOI: 10.3390/cells10123397. [14] AWASTHI D, CHOPRA S, CHO B A, et al. Inflammatory ER stress responses dictate the immunopathogenic progression of systemic candidiasis[J]. J Clin Invest, 2023, 133(17): e167359. DOI: 10.1172/JCI167359. [15] WRON ' SKA A K, KACZMAREK A, SOBICH J, et al. The effect of infection with the entomopathogenic fungus Conidiobolus coronatus (Entomopthorales) on eighteen cytokine-like proteins in Galleria mellonella (Lepidoptera) larvae[J]. Front Immunol, 2024, 15: 1385863. DOI: 10.3389/fimmu.2024.1385863. [16] 崔文佳, 温慧灵, 田荣华, 等. COPD患者继发真菌感染与血清PLT及IL-2水平的相关性[J]. 西部医学, 2021, 33(6): 882-886.CUI W J, WEN H L, TIAN R H, et al. Secondary fungal infection in COPD patients and its relationship with serum PLT and IL-2 levels[J]. Medical Journal of West China, 2021, 33(6): 882-886. [17] 王中原. 血常规指标和炎症因子水平与慢性阻塞性肺疾病继发真菌感染的关系[J]. 中国微生态学杂志, 2021, 33(9): 1073-1077.WANG Z Y. Relationship of levels of routine blood biochemical indexes and inflammatory factors with secondary fungal infection in COPD[J]. Chinese Journal of Microecology, 2021, 33(9): 1073-1077. [18] CHRISTENSON S A, SMITH B M, BAFADHEL M, et al. Chronic obstructive pulmonary disease[J]. Lancet, 2022, 399(10342): 2227-2242. doi: 10.1016/S0140-6736(22)00470-6 [19] AKSOY E, YILDIRIM E, OZMEN I, et al. Clinical features, treatment outcome and potential risk factors for recurrence among patients with chronic pulmonary aspergillosis in a resource-limited setting: a retrospective observational study[J]. Mycopathologia, 2024, 189(5): 76. DOI: 10.1007/s11046-024-00884-9. [20] MOLINOS-CASTRO S, PESQUEIRA-FONTÁN P M, RODRÍGUEZ-FERNÁNDEZ S, et al. Clinical factors associated with pulmonary aspergillosis in patients with chronic obstructive pulmonary disease[J]. Enferm Infecc Microbiol Clin (Engl Ed), 2020, 38(1): 4-10. doi: 10.1016/j.eimc.2019.06.007 [21] GUO L, WU X L, WU X L. Aspergillus infection in chronic obstructive pulmonary diseases[J]. Clin Respir J, 2023, 17(3): 129-138. doi: 10.1111/crj.13585 [22] MOLINENGO L, ESTRIN-SERLUI T, HANLEY B, et al. Infectious diseases and the role of needle biopsy post-mortem[J]. Lancet Microbe, 2024, 5(7): 707-716. doi: 10.1016/S2666-5247(24)00044-2 [23] WEI L Y, LUO J Y, WU W W, et al. Clinical diagnostic value of metagenomic next-generation sequencing in patients with acute infection in emergency department[J]. Heliyon, 2024, 10(16): e35802. DOI: 10.1016/j.heliyon.2024.e35802. [24] HILT E E, FERRIERI P. Next Generation and other sequencing technologies in diagnostic microbiology and infectious diseases[J]. Genes (Basel), 2022, 13(9): 1566. DOI: 10.3390/genes13091566. [25] MIAO Q, MA Y Y, WANG Q, et al. Microbiological diagnostic performance of metagenomic next-generation sequencing when applied to clinical practice[J]. Clin Infect Dis, 2018, 67(suppl_2): S231-S240. doi: 10.1093/cid/ciy693 -





 下载:
下载: