The prognostic value of systemic immune-inflammation index and fibrinogen to prealbumin ratio in prostate cancer
-
摘要:
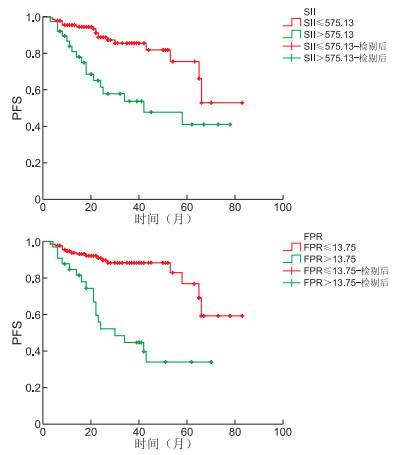
目的 探讨系统免疫炎症指数(SII)及纤维蛋白原与前白蛋白比值(FPR)在前列腺癌患者中的预后价值,以期为术后患者的转归提供依据。 方法 以2014年1月—2020年9月在蚌埠医科大学第二附属医院泌尿外科行前列腺癌根治术(RP)的175例患者为研究对象,收集患者相关临床资料和随访信息。利用ROC曲线明确SII和FPR的最佳截断值,分为高SII组和低SII组、高FPR组和低FPR组,分析不同SII、FPR分组的前列腺癌患者临床病理特征,同时建立Kaplan-Meier曲线对PFS和OS进行分析,采用Cox比例风险模型分析影响前列腺癌预后的危险因素。 结果 SII和FPR的截断值分别为575.13、13.75。不同SII分组患者切缘阳性状况、术后病理分期和不同FPR分组患者精囊侵犯情况、切缘阳性状况比较,差异均有统计学意义(P<0.05)。生存分析显示,低SII组、低FPR组患者术后3、5年PFS和OS分别高于高SII组、高FPR组。与SII联合FPR 0、1分组相比,2分组的5年PFS和OS最低,差异有统计学意义(P < 0.001)。多因素分析表明,术前tPSA、SII、FPR是影响患者PFS的独立预后因素;切缘状况、SII、FPR是影响OS的独立预后因素。 结论 SII和FPR均可作为预测前列腺癌患者的预后指标,二者联合预测的准确性更佳。 -
关键词:
- 前列腺癌 /
- 系统免疫炎症指数 /
- 纤维蛋白原与前白蛋白比值 /
- 预后
Abstract:Objective To investigate the prognostic value of the systemic immune-inflammation index (SII) and fibrinogen to prealbumin ratio (FPR) in patients with prostate cancer, so as to provide evidence for the outcome of postoperative patients. Methods A total of 175 patients who underwent radical prostatectomy (RP)in the Department of Urology, the Second Affiliated Hospital of Bengbu Medical University from January 2014 to September 2020 were enrolled as subjects, and the relevant clinical data and follow-up information were collected. The optimal cut-off values of SII and FPR were determined using the ROC curves. Based on these cut-offs, patients were divided into high and low SII groups, and high and low FPR groups. The clinicopathological features of prostate cancer patients with different SII and FPR groups were analyzed, and Kaplan-Meier curves were established to analyze the PFS and OS. The Cox proportional hazards model was used to analyze the risk factors for PFS and OS of prostate cancer. Results The cut-off values of SII and FPR were 575.13 and 13.75, respectively. There were statistically significant differences in positive margin status, postoperative pathological stage among patients with different SII groups, and seminal vesicle invasion and positive margin status among patients with different FPR groups (P < 0.05). Survival analysis showed that PFS and OS in the low SII group and low FPR group were higher than those in the high SII group and high FPR group at 3 and 5 years after surgery, respectively. Compared with the combination of SII and FPR 0 and 1 groups, the 5-year PFS and OS of group 2 were the lowest, and the difference was statistically significant (P < 0.001). Multivariate analysis showed that preoperative tPSA, SII, and FPR were independent prognostic factors affecting PFS; margin status, SII, and FPR were independent prognostic factors affecting OS. Conclusion Both SII and FPR can be used as prognostic indicators for patients with prostate cancer, and the combination of the two has better predictive accuracy. -
表 1 高、低FPR组间和高、低SII组间PCa患者临床资料比较
Table 1. Comparison of clinical characteristics between high and low FPR groups and between high and low SII groups in patients with PCa
项目 高FPR组(n=33) 低FPR组(n=142) 统计量 P值 高SII组(n=38) 低SII组(n=137) 统计量 P值 年龄(x±s,岁) 71.39±6.10 69.36±6.33 0.165a 0.101 71.45±5.82 69.27±6.51 0.864a 0.064 吸烟史[例(%)] 0.245b 0.621 1.171b 0.279 是 9(27.3) 45(31.7) 9(23.7) 45(32.8) 否 24(72.7) 97(68.3) 29(76.3) 92(67.2) 高血压史[例(%)] 0.321b 0.571 0.440b 0.507 是 19(57.6) 74(52.1) 22(57.9) 71(51.8) 否 14(42.4) 68(47.9) 16(42.1) 66(48.2) 糖尿病史[例(%)] 0.076b 0.782 0.409b 0.522 是 6(18.2) 23(16.2) 5(13.2) 24(17.5) 否 27(81.8) 119(83.8) 33(86.8) 113(82.5) Gleason评分[例(%)] 2.247b 0.134 1.098b 0.295 < 8分 16(48.5) 89(62.7) 20(52.6) 85(62.0) ≥8分 17(51.5) 53(37.3) 18(47.4) 52(38.0) 术前tPSA(x±s,μg/L) 22.94±15.17 21.55±17.90 0.412a 0.681 22.94±15.17 21.55±17.89 0.412a 0.681 切缘阳性状况[例(%)] 5.467b 0.019 6.262b 0.012 是 14(42.4) 32(22.5) 16(42.1) 30(21.9) 否 19(57.6) 110(77.5) 22(57.9) 107(78.1) 脉管神经侵犯[例(%)] 0.239b 0.625 1.529b 0.216 是 9(27.3) 33(23.2) 12(31.6) 30(21.9) 否 24(72.7) 109(76.8) 26(68.4) 107(78.1) 淋巴结阳性[例(%)] 2.763b 0.096 0.015b 0.902 是 7(21.2) 15(10.6) 5(13.2) 17(12.4) 否 26(78.8) 127(89.4) 33(86.8) 120(87.6) 精囊侵犯[例(%)] 12.050b 0.002 3.502b 0.061 是 11(33.3) 14(9.9) 9(23.7) 16(11.7) 否 22(66.7) 128(90.1) 29(76.3) 121(88.3) 病理分期[例(%)] 2.415b 0.120 4.811b 0.028 T2 21(63.6) 109(76.8) 23(60.5) 107(78.1) T3~4 12(36.4) 33(23.2) 15(39.5) 30(21.9) 注:a为t值,b为χ2值。 表 2 前列腺癌术后生存预后单因素分析
Table 2. Univariate analysis of postoperative survival prognosis in prostate cancer
变量 PFS OS HR(95% CI) P值 HR(95% CI) P值 术前tPSA 2.740(1.342~5.595) 0.006 3.868(1.076~13.903) 0.038 Gleason评分 2.006(1.029~3.911) 0.041 4.706(1.473~15.038) 0.009 切缘情况 2.232(1.110~4.485) 0.024 13.930(3.802~51.035) <0.001 精囊侵犯 3.496(1.705~7.171) 0.001 5.350(1.852~15.461) 0.002 病理分期 1.810(0.098~3.607) 0.092 7.684(2.405~24.547) 0.001 SII 3.736(1.923~7.260) < 0.001 5.714(1.912~17.077) 0.002 FPR 5.216(2.670~10.188) < 0.001 7.330(2.290~23.459) 0.001 表 3 前列腺癌术后生存预后多因素分析
Table 3. Multivariate analysis of postoperative survival prognosis of prostate cancer
变量 PFS OS HR(95% CI) P值 HR(95% CI) P值 术前tPSA 2.204(1.046~4.646) 0.038 1.290(0.288~5.781) 0.740 切缘情况 1.018(0.469~2.208) 0.964 4.792(1.080~21.259) 0.039 SII 2.721(1.286~5.758) 0.009 7.643(1.976~29.560) 0.003 FPR 2.718(1.196~6.176) 0.017 4.417(1.220~15.987) 0.024 -
[1] BRAY F, LAVERSANNE M, SUNG H, et al. Global cancer statistics 2022: Globocan estimates of incidence and mortality worldwide for 36 cancers in 185 countries[J]. CA Cancer J Clin, 2024, 74(3): 229-263. [2] SEKHOACHA M, RIET K, MOTLOUNG P, et al. Prostate cancer review: genetics, diagnosis, treatment options, and alternative approaches[J]. Molecules, 2022, 27(17): 5730. DOI: 10.3390/molecules27175730. [3] HUANG Y H, CHEN Y, ZHU Y, et al. Postoperative systemic immune-inflammation index (SII): a superior prognostic factor of endometrial cancer[J]. Front Surg, 2021, 8: 704235. DOI: 10.3389/fsurg.2021.704235. [4] ZHENG J X, PENG L, ZHANG S H, et al. Preoperative systemic immune-inflammation index as a prognostic indicator for patients with urothelial carcinoma[J]. Front Immunol, 2023, 14: 1275033. DOI: 10.3389/fimmu.2023.1275033. [5] 李静, 刘继斌, 江晓晖, 等. 术前纤维蛋白原-前白蛋白比值联合血小板-淋巴细胞比值评分对结直肠癌根治性切除术患者的预后评估价值[J]. 肿瘤学杂志, 2024, 30(6): 467-476.LI J, LIU J B, JIANG X H, et al. Prognostic value of preoperative fibrinogen-to-prealbumin ratio combined with platelet-to-lymphocyte ratio score in patients undergoing radical resection of colorectal cancer[J]. Journal of Chinese Oncology, 2024, 30(6): 467-476. [6] 黄琴, 蒿艳蓉, 吕艳茹, 等. 系统免疫炎症指数, 纤维蛋白原与白蛋白比值对晚期肺癌一线化疗患者预后的影响[J]. 广西医科大学学报, 2023, 40(8): 1321-1328.HUANG Q, HAO Y R, LYU Y R, et al. Effects of systemic immune-inflammation index and fibrinogen to albumin ratio on the prognosis of patients with advanced lung cancer receiving first-line chemotherapy[J]. Journal of Guangxi Medical University, 2023, 40(8): 1321-1328. [7] XIE H L, HUANG S Z, YUAN G H, et al. Prognostic significance of preoperative fibrinogen-to-prealbumin ratio in patients with stage Ⅰ-Ⅲ colorectal cancer undergoing surgical resection: a retrospective cohort study[J]. Biomed Res Int, 2021, 2021: 3905353. DOI: 10.1155/2021/3905353. [8] KANNO H, HISAKA T, AKIBA J, et al. C-reactive protein/albumin ratio and Glasgow prognostic score are associated with prognosis and infiltration of Foxp3+ or CD3+ lymphocytes in colorectal liver metastasis[J]. BMC Cancer, 2022, 22(1): 839. DOI: 10.1186/s12885-022-09842-4. [9] HIBINO S, KAWAZOE T, KASAHARA H. et al. Inflammation-induced tumorigenesis and metastasis[J]. Int J Mol Sci, 2021, 22(11): 5421. DOI: 10.3390/ijms22115421. [10] BAE B K, PARK H C, YOO G S, et al. The significance of systemic inflammation markers in intrahepatic recurrence of early-stage hepatocellular carcinoma after curative treatment[J]. Cancers (Basel), 2022, 14(9): 2081. DOI: 10.3390/cancers14092081. [11] NOST T H, ALCALA K, URBAROVA I, et al. Systemic inflammation markers and cancer incidence in the UK Biobank[J]. Eur J Epidemiol, 2021, 36(8): 841-848. doi: 10.1007/s10654-021-00752-6 [12] LUO Z M, WANG W, XIANG L Y, et al. Association between the systemic immune-inflammation index and prostate cancer[J]. Nutr Cancer, 2023, 75(10): 1918-1925. doi: 10.1080/01635581.2023.2272800 [13] WANG S, YANG X, YU Z Y, et al. The values of systemic immune-inflammation index and neutrophil-lymphocyte ratio in predicting biochemical recurrence in patients with localized prostate cancer after radicalprostatectomy[J]. FrontOncol, 2022, 12: 907625. DOI: 10.3389/fonc.2022.907625. [14] MENG L H, YANG Y J, HU X, et al. Prognostic value of the pretreatment systemic immune-inflammation index in patients with prostate cancer: a systematic review and meta-analysis[J]. J Transl Med, 2023, 21(1): 79. DOI: 10.1186/s12967-023-03924-y. [15] ZHANG B W, XU T. Prognostic significance of pretreatment systemic immune-inflammation index in patients with prostate cancer: a meta-analysis[J]. World J Surg Oncol, 2023, 21(1): 2. DOI: 10.1186/s12957-022-02878-7. [16] WU X Y, YU X M, CHEN C, et al. Fibrinogen and tumors[J]. Front Oncol, 2024, 14: 1393599. DOI: 10.3389/fonc.2024.1393599. [17] MITSUI S, TANAKA Y, DOIT, et al. Prognostic value of preoperative plasma fibrinogen levels in resected stage I non-small cell lung cancer[J]. Thorac Cancer, 2022, 13(10): 1490-1495. doi: 10.1111/1759-7714.14419 [18] YE X W, HU H J, XIONG X Z, et al. The preoperative elevated plasma fibrinogen level is associated with the prognosis of hilar cholangiocarcinoma[J]. Surg Today, 2021, 51(8): 1352-1360. doi: 10.1007/s00595-021-02249-x [19] LEI X, ZHANG T F, DENG Z X, et al. Coagulation markers as independent predictors of prostate cancer aggressiveness: a retrospective cohort study[J]. Sci Rep, 2023, 13(1): 16073. DOI: 10.1038/s41598-023-43427-w. [20] 潘文, 吕彦天, 张中伟, 等. 术前C反应蛋白与白蛋白比值对非小细胞肺癌患者预后的预测价值[J]. 医学研究杂志, 2023, 52(10): 150-154.PAN W, LYU Y T, ZHANG Z W, et al. Prognostic value of preoperative C-reactive protein to albumin ratio in patients with non-small cell lung cancer[J]. Journal of Medical Research, 2023, 52(10): 150-154. [21] 马勇, 陈善勤, 傅军等. 血清纤维蛋白原及白蛋白/球蛋白比值水平与胃癌患者生存预后的关系[J]. 中华全科医学, 2023, 21(6): 945-949. doi: 10.16766/j.cnki.issn.1674-4152.003021MA Y, CHEN S Q, FU J, et al. Relationship between serum fibrinogen and albumin/globulin ratio and survival prognosis of patients with gastric cancer[J]. Chinese Journal of General Practice, 2023, 21(6): 945-949. doi: 10.16766/j.cnki.issn.1674-4152.003021 [22] LI H W, SUN Y F, WANG C, et al. Prognostic value of fibrinogen to prealbumin ratio (FPR) in resectable gastric cancer[J]. J Inflamm Res, 2024, 17: 1325-1335. doi: 10.2147/JIR.S440832 [23] 刘北, 夏海龙, 焦燕, 等. 纤维蛋白原/前白蛋白比值与多发性骨髓瘤患者预后的关系[J]. 医学信息, 2024, 37(1): 130-134.LIU B, XIA H L, JIAO Y, et al. Relationship between fibrinogen/prealbumin ratio and prognosis of patients with multiple myeloma[J]. Medical Information, 2024, 37(1): 130-134. [24] 杜晓平, 邱根祥, 许宝才, 等. 血清前白蛋白/纤维蛋白原比值与胃癌临床病理特征及预后的关系研究[J]. 浙江中西医结合杂志, 2021, 31(4): 332-334.DU X P, QIU G X, XU B C, et al. Relationship between serum prealbumin/fibrinogen ratio and clinicopathological features and prognosis of gastric cancer[J]. Zhejiang Journal of Integrated Traditional Chinese and Western Medicine, 2021, 31(4): 332-334. [25] 李建华, 王志杰, 武玉东. 系统免疫炎症指数联合白蛋白-纤维蛋白原比值对初诊前列腺癌患者骨转移的预测价值[J]. 肿瘤基础与临床, 2024, 37(1): 17-20.LI J H, WANG Z J, WU Y D. Predictive value of systemic immune-inflammation index combined with albumin-fibrinogen ratio for bone metastasis in patients with newly diagnosed prostate cancer[J]. Journal of Basic and Clinical Oncology, 2024, 37(1): 17-20. -





 下载:
下载: