The mediating role of self-efficacy and family support in the relationship between illness perception and treatment adherence in patients with major depressive disorder
-
摘要:
目的 基于横断面调查数据,分析重度抑郁症(MDD)患者治疗依从性的现状,并验证自我效能和家庭支持在疾病感知与治疗依从性之间的中介作用模型。 方法 通过便利抽样法,纳入2022年8月—2024年8月绍兴市第七人民医院收治的160例MDD患者,选用一般自我效能量表(GSES)、Morisky用药依从性量表(MMAS-8)等进行问卷调查。自我效能和家庭支持在MDD患者疾病感知与治疗依从性间的中介作用选用Process插件进行分析。 结果 本研究收回156份(97.50%)有效问卷,MMAS-8评分为(5.72±1.36)分。Pearson相关系数分析显示,MMAS-8评分与GSES、家庭支持评分均呈正相关关系(r=0.658、0.514,P<0.001)。Bootstrap检验结果显示,间接效应值为-0.152(95% CI:-0.216~-0.107),直接效应值为-0.233(95% CI:-0.308~-0.112)。 结论 MDD患者治疗依从性有待提高,疾病感知可直接影响患者的治疗依从性,还可通过自我效能和家庭支持间接影响患者的治疗依从性。 Abstract:Objective To analyze the current status of treatment compliance in patients with major depressive disorder (MDD) and to validate the mediating model of self-efficacy and family support between illness perception and treatment compliance, based on cross-sectional survey data. Methods A total of 160 patients with MDD admitted to Shaoxing 7th People' s Hospital from August 2022 to August 2024 were selected by a convenience sampling method, and the general self-efficacy scale (GSES) and Morisky medical adherence scale (MMAS-8) were used for a questionnaire survey. The mediating role of self-efficacy and family support between disease perception and treatment compliance of MDD patients was analyzed through the Process plug-in. Results The MMAS-8 score of 156 (97.50%) valid questionnaires collected in this study was (5.72±1.36) points. Pearson correlation coefficient analysis showed that the MMAS-8 score was positively correlated with GSES and family support score (r=0.658, 0.514, P < 0.001). Bootstrap test showed that the indirect effect value was -0.152 (95% CI: -0.216 to -0.107) and the direct effect value was -0.233 (95% CI: -0.308 to -0.112). Conclusion The treatment compliance of patients with MDD needs to be improved. Disease perception can directly affect the treatment compliance of patients, and it can also indirectly affect the treatment compliance of patients through self-efficacy and family support. -
Key words:
- Depression /
- Disease perception /
- Compliance /
- Self-efficacy /
- Family support /
- Intermediary function
-
表 1 不同人口学特征MDD患者MMAS-8评分比较(x±s,分)
Table 1. Comparison of MMAS-8 scores of MDD patients with different demographic characteristics (x±s, points)
项目 例数 MMAS-8评分 统计量 P值 性别 0.267a 0.790 男性 95 5.69±1.32 女性 61 5.75±1.40 年龄(岁) 0.279a 0.781 ≤40 82 5.68±1.33 >40 74 5.74±1.35 起病年龄(岁) 3.886b 0.023 ≤30 51 5.47±1.03 >30~44 43 5.71±1.34 ≥45 62 6.14±1.48 病程(月) 0.137a 0.891 <14 69 5.70±1.38 ≥14 87 5.73±1.32 文化水平 8.739b <0.001 初中及以下 21 4.97±1.45 高中及大专 46 5.69±1.31 本科及以上 89 6.21±1.28 婚姻状态 0.141a 0.888 已婚 88 5.74±1.37 未婚/丧偶/离异 68 5.71±1.28 工作状态 0.971a 0.334 在职 109 5.83±1.42 未在职 47 5.60±1.33 精神病家族史 0.832a 0.411 是 27 5.58±1.43 否 129 5.83±1.37 家庭月平均收入(元) 4.899b 0.009 ≤3 000 36 5.29±1.17 3 001~5 000 71 5.85±1.28 ≥5 001 49 6.18±1.41 近2年发作次数(次) 1.219b 0.298 0 38 5.62±1.35 1 77 5.89±1.38 2 41 5.51±1.27 最近一次发作时长(月) 2.637b 0.075 ≤2 79 6.03±1.44 >2~<12 34 5.73±1.41 ≥12 43 5.42±1.37 注:a为t值,b为F值。 表 2 MDD患者自我效能、家庭支持与疾病感知、治疗依从性的相关性
Table 2. Correlation between self-efficacy, family support, disease perception and treatment compliance of MDD patients
项目 GSES评分 家庭支持评分 r值 P值 r值 P值 BIPQ评分 -0.427 <0.001 -0.386 <0.050 MMAS-8评分 0.658 <0.001 0.514 <0.001 表 3 Bootstrap中介效应检验结果
Table 3. Results of bootstrap mediation analysis
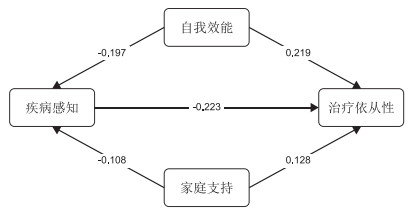
影响路径 效应值 95% CI P值 占比(%) 疾病感知→自我效能→治疗依从性 -0.115 -0.204~-0.076 <0.001 30.67 疾病感知→家庭支持→治疗依从性 -0.037 -0.143~-0.005 <0.050 9.86 间接效应 -0.152 -0.216~-0.107 <0.050 40.53 直接效应 -0.223 -0.308~-0.112 <0.001 59.47 总效应 -0.375 -0.421~-0.184 <0.001 100.00 -
[1] CHEN X, CHEN Y, ZHOU L, et al. The role of self-esteem as moderator of the relationship between experienced stigma and anxiety and depression among tuberculosis patients[J]. Sci Rep, 2023, 13(1): 6889. DOI: 10.1038/s41598-023-34129-4. [2] GU X, SHEN X, CHU J H, et al. Frailty, illness perception and lung functional exercise adherence in lung cancer patients after thoracoscopic surgery[J]. Patient Prefer Adherence, 2023, 17(1): 2773-2787. [3] 任鹏娜, 张月, 丁琳, 等. 运动恐惧在急性心肌梗死经皮冠状动脉介入治疗术后患者自我效能与运动依从性间的中介效应[J]. 解放军护理杂志, 2022, 39(1): 21-24.REN P N, ZHANG Y, DING L, et al. Mediating effect of exercise fear on self-efficacy and exercise compliance of patients with acute myocardial infarction after percutaneous coronary intervention[J]. Military Nursing, 2022, 39(1): 21-24. [4] 崔艳丽, 范丽娟, 张玲玲. 恶性肿瘤患者知情程度与治疗依从性的关系: 心理状态和家庭社会支持的中介作用分析[J]. 现代医学, 2023, 51(3): 328-333.CUI Y L, FAN L J, ZHANG L L. The relationship between the degree of knowledge and treatment compliance of patients with malignant tumor: an analysis of the mediating role of psychological state and family social support[J]. Modern Medical Journal, 2023, 51(3): 328-333. [5] LIU Y R, WANG Y, LIU J, et al. Path analysis of illness perception, medication beliefs, family support on inhaler adherence in elderly COPD patients: based on triadic reciprocal determinism[J]. Patient Educ Couns, 2025, 130(1): 108465. DOI: 10.1016/j.pec.2024.108465. [6] 中华医学会精神病学分会. 中国精神障碍分类与诊断标准第三版(精神障碍分类)[J]. 中华精神科杂志, 2001, 34(3): 184-188.Psychiatry Branch of Chinese Medical Association. China Classification and Diagnostic Criteria for Mental Disorders Third Edition (Classification of Mental Disorders)[J]. Chinese Journal of Psychiatry, 2001, 34(3): 184-188. [7] 孙丽丽, 胡伟, 范秋瑾, 等. 丁螺环酮联合米氮平与正念认知疗法对高血压合并抑郁症患者血压、HAMD17评分的影响[J]. 中南医学科学杂志, 2022, 50(5): 758-761.SUN L L, HU W, FAN Q J, et al. Effects of buspirone combined with mirtazapine and mindfulness cognitive therapy on blood pressure and HAMD17 score in patients with hypertension complicated with depression[J]. Medical Science Journal of Central South China, 2022, 50(5): 758-761. [8] 陈维尔, 邱艳, 潘晓华, 等. 高血压共病糖尿病患者服药依从性调查及影响因素分析[J]. 中华全科医学, 2024, 22(4): 601-604.CHEN W E, QIU Y, PAN X H, et al. Investigation on medication compliance of patients with hypertension and diabetes mellitus and analysis of influencing factors[J]. Chinese Journal of General Practice, 2024, 22(4): 601-604. [9] 王静, 丁劲, 苏晶, 等. 中青年原发性高血压患者疾病感知与自我管理行为的相关性研究[J]. 心理月刊, 2022, 17(16): 231-233.WANG J, DING J, SU J, et al. Correlation between disease perception and self-management behavior in young and middle-aged patients with essential hypertension[J]. Psychologies Magazine, 2022, 17(16): 231-233. [10] SCHWARZER R, BAESSLER J, KWIATEK P, et al. The assessment of optimistic self-beliefs: comparison of the German, Spanish, and Chinese versions of the general self-efficacy scale[J]. Appl Psychol Int Rev, 1997, 46(1): 69-88 [11] 许嘉乐, 傅利勤, 吴红, 等. 康复自我效能在髋/膝关节置换术后住院患者领悟社会支持与康复锻炼依从性间的中介作用[J]. 上海交通大学学报(医学版), 2024, 44(8): 959-967.XU J L, FU L Q, WU H, et al. The mediating role of rehabilitation self-efficacy between inpatients ' perception of social support and compliance with rehabilitation exercise after hip/knee replacement[J]. Journal of Shanghai Jiaotong University(Medical Science), 2024, 44(8): 959-967. [12] CHIN T, HUYGHEBAERT T, SVRCEK C, et al. Individualized antidepressant therapy in patients with major depressive disorder: novel evidence-informed decision support tool[J]. Can Fam Physician, 2022, 68(11): 807-814. doi: 10.46747/cfp.6811807 [13] ZAIBI H, ALLOUCHE A, BEN JEMIA E, et al. Assessment of therapeutic compliance and its associated factors in tunisian adult asthmatic patients[J]. Tunis Med, 2023, 101(2): 266-272. [14] 周俊超. 重度抑郁症患者联合用药治疗无效的影响因素分析[J]. 河北医药, 2021, 43(7): 1047-1050.ZHOU J C. Analysis of influencing factors of ineffective combined medication in patients with severe depression[J]. Hebei Medical Journal, 2021, 43(7): 1047-1050. [15] 崔海艳, 景涛, 邹新亮, 等. 急性心肌梗死患者PCI后服药依从性较差的主要影响因素及其BP神经网络模型构建[J]. 实用心脑肺血管病杂志, 2024, 32(6): 45-50.CUI H Y, JING T, ZOU X L, et al. The main influencing factors of poor drug compliance in patients with acute myocardial infarction after PCI and the construction of BP neural network model[J]. Practical Journal of Cardiac Cerebral Pneumal and Vascular Disease, 2024, 32(6): 45-50. [16] 韦丽鹤, 王纳, 薛娜, 等. 基于保护动机理论的健康教育对进展期胃癌患者服药行为、负性心理反应和疾病感知的影响[J]. 中国健康心理学杂志, 2022, 30(3): 372-377.WEI L H, WANG N, XUE N, et al. Effects of health education based on protective motivation theory on medication behavior, negative psychological reaction and disease perception of patients with advanced gastric cancer[J]. China Journal of Health Psychology, 2022, 30(3): 372-377. [17] 陈洁瑶, 方亚, 曾雁冰. 多元社会参与及家庭支持对中国老年人心理健康的影响研究[J]. 中国卫生政策研究, 2021, 14(10): 45-51.CHEN J Y, FANG Y, ZENG Y B. Study on the influence of multi-social participation and family support on the mental health of the elderly in China[J]. Chinese Journal of Health Policy, 2021, 14(10): 45-51. [18] CHEN Q, LIANG C, ZHAO Y, et al. The mediating role of coping styles in illness perception and self-management in patients with obstructive sleep apnea[J]. Sleep Med, 2024, 113(1): 349-356. -





 下载:
下载: