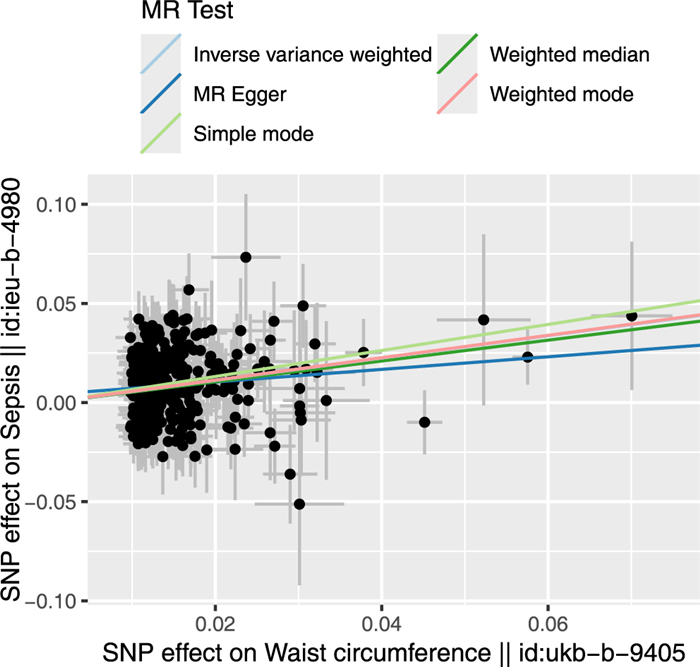
Causal relationship between increased waist circumference and sepsis based on bidirectional two-sample Mendelian randomization analysis
-
摘要:
目的 使用两样本孟德尔随机化分析,探讨腰围与脓毒症之间的潜在因果关系,为临床精准识别中心性肥胖人群中的高风险个体、制定感染性疾病的预防与干预策略提供循证依据。 方法 本研究为两样本双向MR设计,暴露变量为腰围(样本量462 166例),结局变量为脓毒症(病例11 643例,对照474 841例),数据均来源于全基因组关联研究(GWAS)数据集,以P<5×10-8、SNP间距离>10 000 kb、r2<0.001为筛选标准,选取腰围相关的单核苷酸多态性(SNP)作为工具变量。主分析方法为逆方差加权法(IVW),辅以MR-Egger回归、加权中位数法、简单模型及加权模型。通过MR-Egger截距检验评估水平多效性,采用“留一法”进行敏感性分析,确保结果的稳定性和可靠性。 结果 MR分析显示腰围与脓毒症在遗传预测上存在显著正向因果关系,IVW分析显示腰围每增加1个标准差,脓毒症的发生风险增加0.753倍(OR=1.753,95% CI:1.571~1.956,P<0.001),多种方法分析结果一致。敏感性分析及多效性检验提示结果稳健,未发现明显的偏倚。性别分层分析显示,男性和女性腰围与脓毒症风险关系一致。反向MR分析未发现脓毒症对腰围存在显著影响。 结论 本研究结果显示腰围增粗可增加脓毒症的发生风险,提示临床上应关注中心性肥胖人群在感染性疾病中的高风险价值,这为脓毒症的预防和管理提供了遗传学层面的新证据。 Abstract:Objective To explore the potential causal relationship between waist circumference and sepsis using a two-sample Mendelian randomization (MR) analysis, providing evidence-based support for the clinical identification of high-risk individuals with central obesity and the development of prevention and intervention strategies for infectious diseases. Methods This study used a two-sample bidirectional Mendelian randomization design. The waist circumference served as the exposure variable (n=462 166), and sepsis was the outcome (11 643 cases and 474 841 controls). Data are sourced from the genome-wide association studies (GWAS) dataset. Single nucleotide polymorphisms (SNPs) associated with waist circumference (P < 5×10-8) and independent of linkage disequilibrium (distance>10 000 kb, r2 < 0.001) were selected as instrumental variables. The inverse variance weighting (IVW) method was used as the primary analytical approach, supplemented with MR-Egger regression, weighted median, simple model, and weighted model analyses. Horizontal pleiotropy was assessed through MR-Egger intercept tests, and sensitivity analysis was conducted using the "leave-one-out" method to ensure the stability and reliability of the results. Results MR analysis showed a significant positive causal relationship between waist circumference and sepsis risk in genetic prediction. The IVW analysis revealed that each standard deviation increase in waist circumference was associated with a 75.3% higher risk of sepsis (OR=1.753, 95% CI: 1.571-1.956, P < 0.001), with consistent results across multiple MR methods. Sensitivity analysis and pleiotropy tests indicated robustness of the findings, with no significant bias. Gender-stratified analysis showed consistent associations between waist circumference and sepsis risk in both men and women. Reverse MR analysis did not identify a significant effect of sepsis on waist circumference. Conclusion This study supports the hypothesis that increased waist circumference may be an independent risk factor for sepsis. These findings underscore the importance of recognizing central obesity as a high-risk condition in populations susceptible to infectious diseases and offer new genetic evidence for the prevention and management of sepsis. -
Key words:
- Sepsis /
- Waist circumference /
- Mendelian randomization /
- Genetic prediction /
- Causal relationship
-
表 1 腰围与脓毒症相关数据信息
Table 1. GWAS summary information on waist circumference and sepsis
数据 人群 病例 对照 总样本量 SNP数量 来源 年份 腰围 European NA NA 462 166 9 851 867 ukb-b-9405 2018 腰围(男性) European NA NA 104 079 2 294 966 ieu-a-71 2015 腰围(女性) European NA NA 127 469 2 473 036 ieu-a-69 2015 脓毒症 European 11 643 474 841 486 484 12 243 539 ieu-b-4980 2021 注:NA表示未提供。 表 2 腰围与脓毒症之间因果关系的MR分析
Table 2. MR analysis of the causal relationship between waist circumference and sepsis
暴露因素 结局因素 MR分析方法 OR值 95% CI P值 F值 腰围 脓毒症 IVW 1.753 1.571~1.956 <0.001 29.794~997.383 MR-Egger回归法 1.374 1.004~1.880 0.047 WM 1.689 1.382~2.065 <0.001 简单模型 1.928 1.148~2.550 0.013 加权模型 1.759 1.214~2.550 0.003 腰围(男性) 脓毒症 IVW 1.031 0.874~1.215 0.719 29.961~86.224 MR-Egger回归法 1.286 0.522~3.166 0.589 WM 1.032 0.819~1.299 0.787 简单模型 0.870 0.552~1.373 0.555 加权模型 1.027 0.688~1.534 0.897 腰围(女性) 脓毒症 IVW 1.107 0.923~1.328 0.272 30.362~130.612 MR-Egger回归法 0.967 0.466~2.004 0.929 WM 1.132 0.869~1.474 0.358 简单模型 1.183 0.742~1.889 0.488 加权模型 1.099 0.737~1.638 0.648 脓毒症 腰围 IVW 1.017 0.999~1.035 0.065 20.914~25.472 MR-Egger回归法 1.024 0.987~1.061 0.210 WM 1.017 0.995~1.040 0.125 简单模型 1.025 0.986~1.066 0.229 加权模型 1.021 0.984~1.060 0.284 -
[1] SINGER M, DEUTSCHMAN C S, SEYMOUR C W, et al. The third international consensus definitions for sepsis and septic shock (sepsis-3)[J]. JAMA, 2016, 315(8): 801-810. doi: 10.1001/jama.2016.0287 [2] LEI S, LI X, ZHAO H, et al. Prevalence of sepsis among adults in China: a systematic review and meta-analysis[J]. Front Public Health, 2022, 10: 977094. DOI: 10.3389/fpubh.2022.977094. [3] LIU Y C, YAO Y, YU M M, et al. Frequency and mortality of sepsis and septic shock in China: a systematic review and meta-analysis[J]. BMC Infect Dis, 2022, 22(1): 564. DOI: 10.1186/s12879-022-07543-8. [4] 谢硕, 李嘉欣, 刘新民, 等. 慢性危重症的特点及预测因素研究进展[J]. 中华全科医学, 2022, 20(9): 1555-1559. doi: 10.16766/j.cnki.issn.1674-4152.002648XIE S, LI J X, LIU X M, et al. Characteristics and predictive factors of chronic critical illness[J]. Chinese Journal of General Practice, 2022, 20(9): 1555-1559. doi: 10.16766/j.cnki.issn.1674-4152.002648 [5] 袁彬珂, 鲁俊. 脓毒症相关危险因素与发病风险及预后关系的孟德尔随机化分析研究进展[J]. 山东医药, 2024, 64(29): 86-90.YUAN B K, LU J. Research progress of Mendelian randomized analysis on the relationship between sepsis-related risk factors and disease risk and prognosis[J]. Shandong Medical Journal, 2024, 64(29): 86-90. [6] 中国居民营养与慢性病状况报告(2020年)[J]. 营养学报, 2020, 42(6): 521.Report on the Nutrition and Chronic Diseases Status of Chinese Residents 2020[J]. Acta Nutrimenta Sinica, 2020, 42(6): 521. [7] BOUTARI C, DEMARSILIS A, MANTZOROS C S. Obesity and diabetes[J]. Diabetes Res Clin Pract, 2023, 202: 110773. DOI: 10.1016/j.diabres.2023.110773. [8] 袁空军, 杨媛, 赵创艺, 等. 腰围、腰围身高比联合体质指数预测血脂异常病人患病风险效果评价[J]. 护理研究, 2022, 36(11): 1894-1900.YUAN K J, YANG Y, ZHAO C Y, et al. Evaluation of the effect of waist circumference, waist-to-height ratio combined with body mass index in predicting the risk of disease in patients with dyslipidemia[J]. Chinese Nursing Research, 2022, 36(11): 1894-1900. [9] 吕垚, 周伊恒, 刘力滴, 等. 美国肥胖医学协会《肥胖和高血压临床实践声明》解读[J]. 中国全科医学, 2025, 28(3): 272-279.LYU Y, ZHOU Y H, LIU L D, et al. Interpretation of the clinical practice statement by the obesity medicine association on the obesity and hypertension[J]. Chinese General Practice, 2025, 28(3): 272-279. [10] WANG Q, SONG X, DU S, et al. Multiple trajectories of body mass index and waist circumference and their associations with hypertension and blood pressure in Chinese adults from 1991 to 2018: a prospective study[J]. Nutrients, 2023, 15(3): 751. DOI: 10.3390/nu15030751. [11] LOU Q. Impact of obesity on outcomes of patients with acute respiratory distress syndrome: a retrospective analysis of a large clinical database[J]. Med Klin Intensivmed Notfmed, 2024, 119(3): 220-226. doi: 10.1007/s00063-023-01042-7 [12] CROUSER E D, CALDWELL C C, HOTCHKISS R S. What is the skinny on obesity during sepsis?[J]. Crit Care Med, 2019, 47(5): 735-736. doi: 10.1097/CCM.0000000000003707 [13] 中华人民共和国国家卫生健康委员会医政司. 肥胖症中国诊疗指南(2024年版)[J]. 协和医学杂志, 2025, 16(1): 90-108.Department of Medical Administration, National Health Commission of the People ' s Republic of China. Chinese guidelines for the clinical management of obesity (2024 edition)[J]. Medical Journal of Peking Union Medical College Hospital, 2025, 16(1): 90-108. [14] 王玉琢, 沈洪兵. 孟德尔随机化研究应用于因果推断的影响因素及其结果解读面临的挑战[J]. 中华流行病学杂志, 2020, 41(8): 1231-1236.WANG Y Z, SHEN H B. Challenges and factors that influencing causal inference and interpretation, based on Mendelian randomization studies[J]. Chinese Journal of Epidemiology, 2020, 41(8): 1231-1236. [15] 王建, 张炎, 程璐, 等. 中性粒细胞胞外诱捕网可增加脓毒症发生风险: 一项两样本单向孟德尔随机化研究[J]. 中华危重病急救医学, 2023, 35(10): 1045-1052.WANG J, ZHANG Y, CHENG L, et al. Neutrophil extracellular trap increase the risk of sepsis: a two-sample, one-way Mendelian randomization study[J]. Chinese Critical Care Medicine, 2023, 35(10): 1045-1052. [16] LU Y, MA J, MA J, et al. Role of obesity in lower mortality risk in sepsis: a meta-analysis of observational studies[J]. Am J Transl Res, 2024, 16(5): 1880-1890. doi: 10.62347/UHBM7298 [17] 张京晓. BMI在脓毒症中的逆流行病学现象及机制研究[D]. 长春: 吉林大学, 2024.ZHANG J X. Study on the countercurrent phenomenon and mechanism of body mass index in sepsis[D]. Changchun: Jilin University, 2024. [18] YEO H J, KIM T H, JANG J H, et al. Obesity paradox and functional outcomes in sepsis: a multicenter prospective study[J]. Crit Care Med, 2023, 51(6): 742-752. doi: 10.1097/CCM.0000000000005801 [19] BUTLER-LAPORTE G, HARROUD A, FORGETTA V, et al. Elevated body mass index is associated with an increased risk of infectious disease admissions and mortality: a Mendelian randomization study[J]. Clin Microbiol Infect, 2021, 27(5): 710-716. doi: 10.1016/j.cmi.2020.06.014 [20] 陈阳. 肥胖脓毒症患者ICU住院时间延长危险因素及预测模型研究[D]. 成都: 西南交通大学, 2022.CHEN Y. Study on risk factors and predictive models for prolonged ICU stay in obese sepsis patients[D]. Chengdu: Southwest Jiaotong University, 2022. [21] LEE Y, AHN S, HAN M, et al. The obesity paradox in younger adult patients with sepsis: analysis of the MIMIC-Ⅳ database[J]. Int J Obes(Lond), 2024, 48(9): 1223-1230. doi: 10.1038/s41366-024-01523-5 [22] PELCZYÑSKA M, MOSZAK M, WESOLEK A, et al. The preventive mechanisms of bioactive food compounds against obesity-induced inflammation[J]. Antioxidants(Basel), 2023, 12(6): 1232. DOI: 10.3390/antiox12061232. [23] 杨丽, 陶玲, 翁翔宇, 等. 肥胖导致的T细胞代谢障碍及相关疾病的研究进展[J]. 现代免疫学, 2024, 44(5): 459-464.YANG L, TAO L, WENG X Y, et al. Research progress of obesity associated T cell metabolic disorder and related diseases[J]. Current Immunology, 2024, 44(5): 459-464. [24] WANG H E, GRIFFIN R, JUDD S, et al. Obesity and risk of sepsis: a population-based cohort study[J]. Obesity(Silver Spring), 2013, 21(12): E762-E769. [25] GURUNATHAN U, RAPCHUK I L, DICKFOS M, et al. Association of obesity with septic complications after major abdominal surgery: a secondary analysis of the RELIEF randomized clinical trial[J]. JAMA Netw Open, 2019, 2(11): e1916345. DOI: 10.1001/jamanetworkopen.2019.16345. -





 下载:
下载: