The effect of syncope on the overall survival after surgery for hepatocellular carcinoma patients
-
摘要:
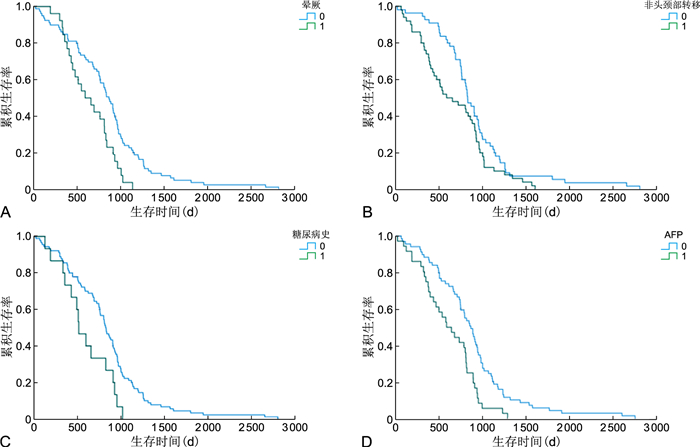
目的 探讨肝细胞肝癌术后1年内发生晕厥与总生存期的关系,为进一步做好肝癌患者的术后管理、提高安宁疗护质量提供参考。 方法 纳入2014年1月—2017年12月就诊于北京天坛医院并接受单纯手术切除肝细胞肝癌的患者,对患者追踪至死亡。收集患者基础资料和术后康复期晕厥发生、肿瘤复发转移等临床资料并进行生存分析,采用Kaplan-Meier法、Cox比例-风险回归模型进行单因素、多因素分析筛选影响总生存期的潜在因素。 结果 105例患者总体中位生存时间为(805.4±45.7)d,主要死因为肝癌。单因素Cox回归分析显示,有糖尿病史、甲胎蛋白水平高、1年内非头颈部转移灶、1年内有晕厥发生、AJCC分期较高均为肝癌术后总生存期的影响因素(P < 0.05)。多因素Cox回归分析显示,甲胎蛋白水平高(OR=1.669,95% CI: 1.031~2.704)、AJCC分期较高(OR=1.322, 95% CI: 1.037~1.685)均为肝癌术后总生存期的独立危险因素。 结论 肝癌术后1年内发生晕厥与肝癌术后总生存期可能有潜在关系,与其他危险因素可能存在交互或间接作用,值得未来在临床中关注。 Abstract:Objective To explore the impact of postoperative syncope on survival of hepatocellular carcinoma (HCC) patients, and aim to provide references for further improving the postoperative management of patients with HCC and the quality of hospice care. Methods HCC patients who underwent surgical resection from January 2014 to December 2017 were included in the study and followed up until death. Basic clinical information and postoperative rehabilitation clinical data were collected for survival analysis, including syncope, distant recurrence and metastasis. The Kaplan-Meier method and the Cox proportional hazards regression model were employed for univariate and multivariate analysis to screen for potential risk factors on overall survival. Results A total of 105 patients were observed until death from HCC, and the overall median survival time was (805.4±45.7) days. Univariate Cox regression analysis demonstrated that the presence of diabetes history, elevated alpha fetoprotein (AFP) levels, distant metastasis within a year, syncope within a year, and higher American Joint Committee on Cancer (AJCC) stage exerted a statistically significant influence on the total survival period after HCC surgery. Multivariate Cox regression analysis demonstrated that elevated AFP value (OR=1.669, 95% CI: 1.031-2.704) and advanced AJCC stage (OR=1.322, 95% CI: 1.037-1.685) were independent risk factors. Conclusion This study hypothesizes that the incidence of syncope in one year has the potential to impact the overall survival of HCC patients post-surgery, and that it may be influenced by other risk factors interactively or indirectly, a factor which requires attention in future research. -
Key words:
- Hepatocellular carcinoma /
- Rehabilitation /
- Overall survival /
- Syncope
-
表 1 HCC患者基本临床资料
Table 1. Basic clinical data of HCC patients
项目 例数(%) 项目 例数(%) 年龄(岁) BUN(mmol/L) ≥60 61(58.1) < 8.3 87(82.9) < 60 44(41.9) ≥8.3 18(17.1) 性别 肌酐(μmol/L) 男性 61(58.1) < 93.3 87(82.9) 女性 44(41.9) ≥93.3 18(17.1) 高血压病史 1年内非头颈部转移灶 无 74(70.5) 无 55(52.4) 有 31(29.5) 有 50(47.6) 糖尿病史 1年内发生晕厥(次) 无 90(85.7) 0 79(75.2) 有 15(14.3) ≥1 26(24.8) AFP(ng/mL) AJCC分期 < 7.0 69(65.7) Ⅰ期 13(12.4) ≥7.0 36(34.3) Ⅱ期 34(32.4) ALT(U/L) Ⅲ期 19(18.1) < 41.0 85(81.0) Ⅳ期 39(37.1) ≥41.0 20(19.0) AST(U/L) < 42.0 85(81.0) ≥42.0 20(19.0) 表 2 肝细胞肝癌患者术后总生存期影响因素的单因素Cox回归分析
Table 2. Univariate Cox regression analysis of factors influencing the overall survival of patients with hepatocellular carcinoma after surgery
变量 B SE Waldχ2 P值 HR值 95% CI 年龄≥60岁 0.248 0.202 1.512 0.219 0.780 0.526~1.159 高血压病史 0.381 0.221 2.967 0.085 0.682 0.442~1.054 糖尿病史 0.726 0.288 6.344 0.012 2.066 1.175~3.634 AFP≥7.0 ng/mL 0.709 0.216 10.808 0.001 2.031 1.331~3.099 ALT≥41.0 U/L 0.110 0.252 0.189 0.663 1.116 0.681~1.830 AST≥42.0 U/L 0.411 0.253 2.629 0.105 1.508 0.918~2.477 BUN≥8.3 mmol/L 0.169 0.261 0.420 0.517 1.184 0.710~1.975 肌酐≥93.3 μmol/L 0.134 0.270 0.248 0.618 0.874 0.515~1.484 1年内非头颈部转移灶 0.404 0.200 4.071 0.044 1.497 1.012~2.216 1年内有发生晕厥 0.690 0.238 8.407 0.004 1.993 1.250~3.177 AJCC分期 0.245 0.091 7.245 0.007 1.278 1.069~1.527 表 3 肝细胞肝癌患者术后总生存期影响因素的多因素Cox回归分析
Table 3. Multivariate Cox regression analyses of factors influencing the overall survival of patients with hepatocellular carcinoma after surgery
临床因素 B SE Waldχ2 P值 HR值 95% CI 糖尿病史 0.330 0.337 0.959 0.328 1.391 0.718~2.695 AFP≥7.0 ng/mL 0.512 0.246 4.335 0.037 1.669 1.031~2.704 1年内非头颈部转移灶 0.239 0.291 0.672 0.412 0.788 0.445~1.394 1年内有发生晕厥 0.375 0.303 1.532 0.216 1.455 0.804~2.634 AJCC分期 0.279 0.124 5.094 0.024 1.322 1.037~1.685 -
[1] BRAY F, LAVERSANNE M, SUNG H, et al. Global cancer statistics 2022: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries[J]. CA Cancer J Clin, 2024, 74(3): 229-263. [2] XIE J, LIN X, FAN X, et al. Global burden and trends of primary liver cancer attributable to comorbid type 2 diabetes mellitus among people living with hepatitis B: an observational trend study from 1990 to 2019[J]. J Epidemiol Glob Health, 2024, 14(2): 398-410. doi: 10.1007/s44197-024-00237-1 [3] DU J S, HSU S H, WANG S N. The current and prospective adjuvant therapies for hepatocellular carcinoma[J]. Cancers(Basel), 2024, 6(7): 1422. DOI: 10.3390/cancers16071422. [4] LORENZEN M O B, FARKAS D K, ADELBORG K, et al. Syncope as a sign of occult cancers: a population-based cohort study[J]. Br J Cancer, 2020, 122(4): 595-600. doi: 10.1038/s41416-019-0692-2 [5] XIE D Y, ZHU K, REN Z G, et al. A review of 2022 Chinese clinical guidelines on the management of hepatocellular carcinoma: updates and insights[J]. Hepatobiliary Surg Nutr, 2023, 12(2): 216-228. doi: 10.21037/hbsn-22-469 [6] 中华心血管病杂志编辑委员会, 中国生物医学工程学会心律分会, 中国老年学和老年医学学会心血管病专业委员会, 等. 晕厥诊断与治疗中国专家共识(2018)[J]. 中华心血管病杂志, 2019, 47(2): 96-107.Editorial Board of Chinese Journal of Cardiology, Heart Rhythm Branch of Chinese Society of Biomedical Engineering, Cardiovascular Diseases Branch of China Association of Gerontology and Geriatrics, et al. Chinese expert consensus statement on clinical diagnosis and treatment of syncope 2018[J]. Chin J Cardiol, 2019, 47(2): 96-107. [7] AKSU T, BRIGNOLE M, CALO L, et al. Cardioneuroablation for the treatment of reflex syncope and functional bradyarrhythmias: a scientific statement of the European Heart Rhythm Association (EHRA) of the ESC, the Heart Rhythm Society (HRS), the Asia Pacific Heart Rhythm Society (APHRS) and the Latin American Heart Rhythm Society (LAHRS)[J]. Europace, 2024, 26(8): euae206. DOI: 10.1093/europace/euae206. [8] HAN B, ZHENG R, ZENG H, et al. Cancer incidence and mortality in China, 2022[J]. J Natl Cancer Cent, 2024, 4(1): 47-53. [9] DUCREUX M, ABOU-ALFA G K, BEKAⅡ-SAAB T, et al. The management of hepatocellular carcinoma. Current expert opinion and recommendations derived from the 24th ESMO/World Congress on Gastrointestinal Cancer, Barcelona, 2022[J]. ESMO Open, 2023, 8(3): 101567. DOI: 10.1016/j.esmoop.2023.101567. [10] MA Y N, JIANG X, SONG P, et al. Neoadjuvant therapies in resectable hepatocellular carcinoma: exploring strategies to improve prognosis[J]. Biosci Trends, 2024, 18(1): 21-41. doi: 10.5582/bst.2023.01436 [11] ZHENG Y, ZHU M, LI M. Effects of alpha-fetoprotein on the occurrence and progression of hepatocellular carcinoma[J]. J Cancer Res Clin Oncol, 2020, 146(10): 2439-2446. doi: 10.1007/s00432-020-03331-6 [12] LI Y C, LI L Y, TONG H C, et al. Pulmonary artery intimal sarcoma mimicking pulmonary thromboembolism: a case report[J]. Medicine(Baltimore), 2021, 100(6): e24699. DOI: 10.1097/MD.0000000000024699. [13] MAGNON C, HONDERMARCK H. The neural addiction of cancer[J]. Nat Rev Cancer, 2023, 23(5): 317-334. doi: 10.1038/s41568-023-00556-8 [14] AMATO M, PIAZZA P, FERRARI I, et al. Rare perinephric myxoid pseudotumor of fat causing ureteropelvic junction obstruction: a case report[J]. CEN Case Rep, 2023, 12(2): 210-214. [15] KHORANA A A, MACKMAN N, FALANGA A, et al. Cancer-associated venous thromboembolism[J]. Nat Rev Dis Primers, 2022, 8(1): 11. DOI: 10.1038/s41572-022-00336-y. [16] YEO Y H, LEE Y T, TSENG H R, et al. Alpha-fetoprotein: past, present, and future[J]. Hepatol Commun, 2024, 8(5): e0422. DOI: 10.1097/HC9.0000000000000422. [17] LIU D, SONG T. Changes in and challenges regarding the surgical treatment of hepatocellular carcinoma in China[J]. Biosci Trends, 2021, 15(3): 142-147. doi: 10.5582/bst.2021.01083 [18] COURI T, PILLAI A. Goals and targets for personalized therapy for HCC[J]. Hepatol Int, 2019, 13(2): 125-137. doi: 10.1007/s12072-018-9919-1 [19] GALLI E, PATELLI G, VILLA F, et al. Circulating blood biomarkers for minimal residual disease in hepatocellular carcinoma: a systematic review[J]. Cancer Treat Rev, 2025, 135: 102908. DOI: 10.1016/j.ctrv.2025.102908. [20] DOMINGUEZ D A, WONG P, MELSTROM L G. Existing and emerging biomarkers in hepatocellular carcinoma: relevance in staging, determination of minimal residual disease, and monitoring treatment response: a narrative review[J]. Hepatobiliary Surg Nutr, 2024, 13(1): 39-55. doi: 10.21037/hbsn-22-526 [21] CHANG Y, WONG C E, LEE P H, et al. Survival outcome of surgical resection vs. radiotherapy in brain metastasis from colorectal cancer: a meta-analysis[J]. Front Med(Lausanne), 2022, 9: 768896. DOI: 10.3389/fmed.2022.768896. [22] 伍龙, 吴欢, 黄飞, 等. 循环肿瘤DNA在结直肠癌中的应用[J]. 中华全科医学, 2024, 22(3): 368-371. doi: 10.16766/j.cnki.issn.1674-4152.003404WU L, WU H, HUANG F, et al. Circulating tumor DNA in colorectal cancer[J]. Chinese Journal of General Practice, 2024, 22(3): 368-371. doi: 10.16766/j.cnki.issn.1674-4152.003404 [23] HO N T, ABE S K, RAHMAN M S, et al. Diabetes is associated with increased liver cancer incidence and mortality in adults: a report from Asia Cohort Consortium[J]. Int J Cancer, 2024, 155(5): 854-870. doi: 10.1002/ijc.34965 [24] SINGH M K, DAS B K, CHOUDHARY S, et al. Diabetes and hepatocellular carcinoma: a pathophysiological link and pharmacological management[J]. Biomed Pharmacother, 2018, 106: 991-1002. doi: 10.1016/j.biopha.2018.06.095 [25] 胡慧英, 张征宇. 运动干预在老年糖尿病周围神经病变患者中的应用效果[J]. 中华全科医学, 2020, 18(5): 769-772. doi: 10.16766/j.cnki.issn.1674-4152.001352HU H Y, ZHANG Z Y. Effect of exercise intervention in elderly patients with diabetic peripheral neuropathy[J]. Chinese Journal of General Practice, 2020, 18(5): 769-772. doi: 10.16766/j.cnki.issn.1674-4152.001352 [26] SUDO S Z, MONTAGNOLI T L, ROCHA B S, et al. Diabetes-induced cardiac autonomic neuropathy: impact on heart function and prognosis[J]. Biomedicines, 2022, 10(12): 3258. DOI: 10.3390/biomedicines10123258. [27] DAS B K, GADAD P C. Impact of diabetes on the increased risk of hepatic cancer: an updated review of biological aspects[J]. Diabetes Epidemiol Manag, 2021, 4: 100025. DOI: 10.1016/j.deman.2021.100025. -





 下载:
下载: