The predictive value of serum albumin changes at 1 year of peritoneal dialysis for the risk of death in peritoneal dialysis patients
-
摘要:
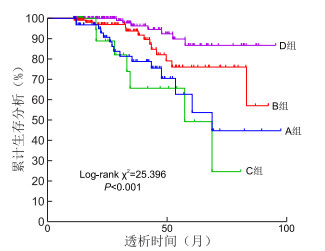
目的 透析前低蛋白血症影响腹膜透析患者生存,白蛋白(ALB)改善对生存率作用的研究较少。本研究结合随访数据,分析腹膜透析1年时ALB变化对患者预后的影响。 方法 回顾分析西安交通大学第一附属医院肾脏内科2015年1月—2019年12月新置管并规律随访超过1年的356例PD患者资料。根据透析前、透析1年时ALB是否≥35 g/L及其变化, 分为持续ALB低水平组(A组,66例)、ALB升高组(B组,113例)、ALB降低组(C组,24例)、持续ALB高水平组(D组,153例)。采用Kaplan-Meier法比较不同组累积生存率,采用Cox风险回归模型评估全因死亡风险。 结果 与透析1年ALB≥35 g/L患者比较,ALB < 35 g/L者肌酐、血红蛋白、握力较低,超敏CRP、腹膜蛋白清除率较高。多因素logistic回归显示,透析初始月高腹膜蛋白清除率(OR=1.023,P < 0.001)、低握力(OR=0.947,P=0.020)、透析1年时高超敏CRP(OR=1.078,P=0.005)、水肿(OR=2.447,P=0.001)均是透析1年时ALB < 35 g/L的独立影响因素。Cox比例风险模型显示,透析1年时ALB < 35 g/L是腹透患者死亡的独立影响因素(OR=3.164,P=0.001)。 结论 透析初始月高腹膜蛋白清除率及低握力,高超敏CRP、水肿是预测透析1年时ALB < 35 g/L的独立危险因素。透析后ALB升高可明显降低腹膜透析患者的死亡风险。 Abstract:Objective Hypoalbuminemia before dialysis affects the survival of peritoneal dialysis (PD) patients, but studies on the effect of albumin improvement on survival rate are limited. This study uses follow-up data to analyze the impact of changes in albumin (ALB) levels after one year of PD on patients ' prognosis. Methods A total of 356 PD patients who underwent new catheterization in the Department of Nephrology, the First Affiliated Hospital of Xi ' an Jiaotong University from January 2015 to December 2019 and received regular follow-up for more than 1 year were retrospectively analyzed. According to their ALB levels at baseline and during one year of dialysis, the patients were divided into continuous low ALB group (group A, n=66), ALB increased group (group B, n=113), ALB decreased group (group C, n=24), and continuous high ALB group (group D, n=153). The Kaplan-Meier method was used to compare the cumulative survival rate among different groups, and the Cox proportional hazards regression model was used to evaluate the risk of all-cause mortality. Results Compared with patients whose ALB ≥35 g/L at 1 year of peritoneal dialysis, those with an ALB level of < 35 g/L had significantly lower creatinine, haemoglobin, and handgrip strength levels, while their high-sensitivity C-reactive protein (hs-CRP) and peritoneal protein clearance levels were significantly higher. Multivariate stepwise logistic regression showed that initial high peritoneal protein clearance rate (OR=1.023, P < 0.001) and low grip strength (OR=0.947, P=0.020), high hs-CRP (OR=1.078, P=0.005), and edema (OR=2.447, P=0.001) were independent influencing factors for albumin < 35 g/L at 1 year of peritoneal dialysis. The Cox proportional hazards model showed that albumin < 35 g/L at 1 year of dialysis was an independent influencing factor for death in peritoneal dialysis patients (OR=3.164, P=0.001). Conclusion High peritoneal protein clearance and low handgrip strength in the first month of peritoneal dialysis, high hs-CRP levels and edema, are independent risk factors for predicting albumin < 35 g/L at 1 year of peritoneal dialysis. An increase in post-dialysis ALB can significantly reduce the mortality risk in peritoneal dialysis patients. -
Key words:
- Peritoneal dialysis /
- Risk of death /
- Albumin /
- Peritoneal protein clearance /
- Handgrip strength
-
表 1 不同白蛋白组PD患者基线资料比较
Table 1. Comparison of baseline data for PD patients in different groups
组别 例数 年龄(x±s,岁) 性别(男性/ 女性, 例) 糖尿病史[例(%)] SBP (x±s,mmHg) DBP (x±s,mmHg) 尿量[M(P25, P75), mL] 尿蛋白定量[M(P25, P75), g/24 h] 白蛋白(x±s,g/L) 血红蛋白(x±s,g/L) AC组 90 53.74±16.37 42/48 24(26.7) 139.51±19.33 82.56±10.81 900.00(627.50, 1 200.00) 1.39(0.53, 1.94) 31.40±5.61 79.76±19.08 BD组 266 46.90±13.74 157/109 45(16.9) 136.99±19.99 84.77±12.16 1 100.00(750.00, 1 500.00) 1.17(0.55, 2.29) 35.32±5.32 84.81±19.34 统计量 3.869a 4.165b 4.091b 0.874a 1.504a -2.728c 0.461c 5.958a 2.097a P值 < 0.001 0.041 0.043 0.305 0.133 0.006 0.984 < 0.001 0.037 组别 例数 尿素[M(P25, P75), mmol/L] 肌酐[M(P25, P75), μmol/L] eGFR[M(P25, P75), mL/(min·1.73m2)] 高/高平均转运比例[例(%)] TKt/V (x±s) TCCr [M(P25, P75), %] PCL [M(P25, P75), mL/d] 握力(x±s, kg) AC组 90 29.53 (21.01, 36.97) 728.10 (588.92, 890.18) 8.05(6.24, 10.69) 36(59.8) 2.15±0.57 78.92 (65.32, 103.43) 69.23 (45.34, 88.14) 19.53±8.96 BD组 266 29.37 (22.51, 36.15) 782.80 (679.95, 930.50) 7.81(6.08, 9.74) 159(40.0) 2.15±0.59 87.65 (67.36, 107.51) 56.18 (39.51, 72.71) 25.10±10.42 统计量 -0.018c -2.562c 1.573c 10.615b 0.017a -1.340c -3.073c 4.154a P值 0.985 0.010 0.116 0.001 0.987 0.180 0.002 < 0.001 注:a为t值,b为χ2值,c为Z值。1 mmHg=0.133 kPa。 表 2 透析1年PD患者生化指标及溶质清除指标比较
Table 2. Comparison of biochemical indicators and solute clearance indicators for PD patients in the first year of peritoneal dialysis
组别 例数 白蛋白(x±s,g/L) 尿素(x±s,mmol/L) 肌酐[M(P25, P75), μmol/L] 血红蛋白(x±s,g/L) 超敏CRP [M(P25, P75), mg/L] rGFR[M(P25, P75), mL/(min·1.73 m2)] AC组 90 31.13±3.78 17.90±6.43 665.50(528.25, 886.00) 95.44±19.69 2.31(0.69,5.98) 2.05(0.59, 4.34) BD组 266 39.79±3.08 18.23±4.69 784.50(615.75, 970.50) 108.35±14.43 1.24(0.50,3.18) 2.56(1.40, 4.21) 统计量 21.425a 0.413a -2.830b 6.600a 1.394b -1.901b P值 < 0.001 0.680 0.005 < 0.001 0.042 0.057 组别 例数 尿量[M(P25, P75), mL] TKt/V (x±s) TCCr [M(P25, P75), %] PCL [M(P25, P75), mL/d] 握力(x±s,kg) AC组 90 525(225, 948) 2.06±0.57 71.30(54.70, 97.13) 83.58(64.18, 83.58) 22.41±9.04 BD组 266 750(400, 1 050) 2.08±0.57 76.75(60.27, 96.87) 53.57(41.43, 66.62) 27.27±9.56 统计量 -2.600b 0.334a -0.795b -7.454b 4.494a P值 0.009 0.739 0.426 < 0.001 < 0.001 注:a为t值,b为Z值。 表 3 透析1年PD患者白蛋白 < 35 g/L风险的多因素logistic回归模型
Table 3. Multivariate stepwise logistic regression model for the risk for PD patients of serum albumin levels below 35 g/L after 12 months of peritoneal dialysis
变量 B SE Waldχ2 P值 OR值 95% CI 透析初始月PCL 0.023 0.006 13.011 < 0.001 1.023 1.011~1.036 透析初始月握力 -0.054 0.023 5.416 0.020 0.947 0.905~0.992 透析1年超敏CRP 0.076 0.027 7.978 0.005 1.078 1.023~1.137 透析1年水肿 0.895 0.259 11.919 0.001 2.447 1.472~4.067 注:将透析1年白蛋白作为因变量,透析1年白蛋白 < 35 g/L=1,透析1年白蛋白≥35 g/L=0;透析初始月握力、PCL、透析1年超敏CRP为连续变量,均以实际值赋值;透析1年水肿为分类变量,有=1,无=0。 表 4 透析1年PD患者白蛋白动态变化的死亡率影响的Cox比例风险模型
Table 4. Cox proportional hazards modelling of the impact of dynamic changes in albumin over one year of dialysis for PD patients
变量 B SE Waldχ2 P值 OR值 95% CI 透析前白蛋白 < 35 g/L 0.412 0.332 1.534 0.216 1.509 0.787~2.896 1年白蛋白 < 35 g/L 1.152 0.310 13.777 0.001 3.164 1.722~5.814 A组 1.782 0.572 9.719 0.002 5.944 1.938~18.227 B组 0.967 0.546 3.137 0.077 2.629 0.902~7.663 C组 1.934 0.526 13.500 < 0.001 6.918 2.466~19.412 注:将是否死亡作为因变量,是=1,否=0。透析前白蛋白 < 35 g/L、1年白蛋白 < 35 g/L=1,否则赋值为0。组间比较时将D组作为对照,OR值设为1,其他各组均与D组进行比较。 表 5 各组PD患者不同时间点握力和PCL比较
Table 5. Comparison of grip strength and PCL in PD patients at different time points in each group
组别 例数 握力(x±s,kg) t值 P值 PCL[M(P25, P75), mL/d] Z值 P值 初始月 透析1年 初始月 透析1年 A组 66 19.03±8.93 20.57±8.83 1.807 0.066 71.73(50.79, 88.14) 85.57(67.42, 110.45) -2.315 0.021 B组 113 24.91±9.15 26.82±9.12 2.259 0.029 66.52(49.82, 86.06) 57.44(43.91, 70.68) -2.538 0.011 C组 24 18.64±8.62 19.45±7.68 1.361 0.619 70.09(48.31, 95.58) 73.98(60.75, 123.45) -1.288 0.198 D组 153 23.98±9.85 25.93±8.63 3.688 < 0.001 49.99(37.02, 67.43) 51.91(37.73, 65.16) -0.147 0.883 -
[1] PITANUPONG J, CHANG A. Relationship of serum albumin at initiation of incident peritoneal dialysis with cardiovascular and overall survival[J]. Clin Nephrol, 2023, 99(6): 265-273. doi: 10.5414/CN110979 [2] HUANG N Y, LI H Y, FAN L, et al. Serum phosphorus and albumin in patients undergoing peritoneal dialysis: interaction and association with mortality[J]. Front Med, 2021, 8: 760394. DOI: 10.3389/fmed.2021.760394. [3] YE H J, LIU R H, CAO P Y, et al. Peritoneal protein clearance, fluid overload, and cardiovascular events in patients undergoing peritoneal dialysis: a prospective cohort study[J]. Ren Fail, 2025, 47(1): 2461676. DOI: 10.1080/0886022X.2025.2461676. [4] 王晓培, 马莹, 吕晶, 等. 腹膜透析患者起始透析剂量对生存率的影响[J]. 临床肾脏病杂志, 2021, 21(11): 904-910.WANG X P, MA Y, LYU J, et al. Effect of initial dialysis dose on survival in peritoneal dialysis patients[J]. Clin Kidney J, 2021, 21(11): 904-910. [5] SHI Y N, CAI J J, SHI C X, et al. Low serum albumin is associated with poor prognosis in patients receiving peritoneal dialysis treatment[J]. J Healthc Eng, 2022, 2022: 7660806. DOI: 10.1155/2022/7660806. [6] 王晓培, 吕晶, 梁嫦娜, 等. 腹膜透析患者营养状态的动态变化与瘙痒及睡眠障碍的关系[J]. 中国血液净化, 2022, 21(10): 719-723.WANG X P, LYU J, LIANG C N, et al. The relationship between the dynamic changes of nutritional status and the symptoms of pruritus and sleep disturbance in peritoneal dialysis patients[J]. Chin J Blood Purif, 2022, 21(10): 719-723. [7] ÇANKAYA E, ALTUNOK M. Comparison of mortality according to baseline, first year, and mean albumin levels in peritoneal dialysis: a retrospective study[J]. Ren Fail, 2023, 45(1): 2176165. DOI: 10.1080/0886022X.2023.2176165. [8] SONG P N, YANG D, LI J E, et al. Dynamic serum albumin and outcome of peritoneal dialysis patients: a retrospective study in China[J]. Front Med, 2022, 9: 917603. DOI: 10.3389/fmed.2022.917603. [9] GUEDES A M. Peritoneal protein loss, leakage or clearance in peritoneal dialysis, where do we stand?[J]. Perit Dial Int, 2019, 39(3): 201-209. doi: 10.3747/pdi.2018.00138 [10] NIU W, YANG X X, YAN H, et al. Peritoneal protein clearance is associated with cardiovascular events but not mortality in peritoneal dialysis patients[J]. Front Med, 2022, 9: 748934. DOI: 10.3389/fmed.2022.748934. [11] YE H J, LIN J X, ZHANG X D, et al. Relationship between peritoneal protein clearance and hemoglobin in peritoneal dialysis patients: a prospective cohort study[J]. J Ren Nutr, 2023, 33(3): 482-489. doi: 10.1053/j.jrn.2023.01.008 [12] 梁嫦娜, 耿瀛洲, 吕晶, 等. 磷清除率对腹膜透析患者血磷及临床转归的影响[J]. 中国血液净化, 2022, 21(3): 177-181.LIANG C N, GENG Y Z, LYU J, et al. Effect of phosphate clearance on serum phosphate and clinical prognosis in peritoneal dialysis patients[J]. Chin J Blood Purif, 2022, 21(3): 177-181. [13] WANG X P, MA Y, LV J, et al. Influence of dietary protein on serum phosphorous levels in peritoneal dialysis patients with different initial transport function[J]. Ren Fail, 2022, 44(1): 2085-2092. doi: 10.1080/0886022X.2022.2148536 [14] 钱宝, 李昭, 吕晶, 等. 腹膜炎对腹透患者营养状况的后续影响[J]. 中国中西医结合肾病杂志, 2023, 24(1): 29-33.QIAN B, LI Z, LYU J, et al. The influence of peritonitis on nutritional status in peritoneal dialysis patients[J]. Chin J Integr Tradit West Nephrol, 2023, 24(1): 29-33. [15] 储安贞, 张兰. 系统免疫炎症指数在川崎病IVIG治疗抵抗患儿中的预测价值[J]. 中华全科医学, 2022, 20(11): 1884-1888. doi: 10.16766/j.cnki.issn.1674-4152.002727CHU A Z, ZHANG L. The predictive value of systemic immune-inflammation index for intravenous immunoglobulin resistance in children with Kawasaki disease[J]. Chin Gen Pract, 2022, 20(11): 1884-1888. doi: 10.16766/j.cnki.issn.1674-4152.002727 [16] 郭洁云, 杨迪, 马慧青, 等. 系统免疫炎症指数在亚急性甲状腺炎中的诊断价值[J]. 中华全科医学, 2025, 23(4): 643-646. doi: 10.16766/j.cnki.issn.1674-4152.003970GUO J Y, YANG D, MA H Q, et al. Diagnostic value of systemic immune-inflammation index in subacute thyroiditis[J]. Chin Gen Pract, 2025, 23(4): 643-646. doi: 10.16766/j.cnki.issn.1674-4152.003970 [17] WILLIAMS J, GILCHRIST M, STRAIN W D, et al. An exploratory study of the relationship between systemic microcirculatory function and small solute transport in incident peritoneal dialysis patients[J]. Perit Dial Int, 2022, 42(5): 513-521. doi: 10.1177/08968608211047332 -





 下载:
下载: